Some women have chronic pain or discomfort in the vulva. This condition is called vulvodynia. No one really knows what causes vulvodynia, but there are treatments that can help relieve the pain. This page explains:
- Causes and symptoms of vulvodynia
- How it is diagnosed
- How is it treated
About Vulvodynia
Vulvodynia is a condition involving chronic pain and discomfort of the vulva. The pain recurs and is long lasting. The two most common types of vulvodynia are:
- Generalized—The pain or discomfort can be felt in the entire vulvar area.
- Localized—Pain is felt only in the vestibule (the opening to the vagina).
With both types, the vulva often looks normal even though a woman feels pain. This pain can affect a woman’s health and her sex life.
Some women with chronic pelvic pain may become afraid to have sex. This fear can lead to vaginismus. This is a spasm of the muscles around the vagina. These spasms may make having sex painful and, in some cases, impossible.
Because chronic pain can make it hard to work or be active, vulvodynia can disrupt a woman’s daily life. Dealing with pain on a long-term basis can cause mental health problems, such as low self-esteem, anxiety, or depression. Emotions and stress also can play a role in how pain is felt and coped with.
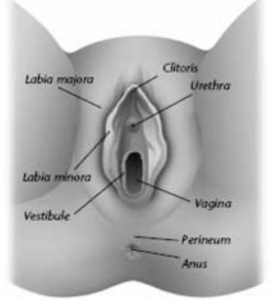
The outside of the female genital area is
called the vulva. The outer lips of the
vulva are called the labia majora. The
inner lips are called the labia minora. The
clitoris is at the top of the inner lips. For
most women, the clitoris is a center of
sexual pleasure. It is partly covered by a
fold of tissue called the hood. The
vestibule is found within the inner lips.
The vagina and the urethra open into the
vestibule. Just inside the vestibule are the
openings to the glands that make
lubrication. The perineum is the area
between the anus and vagina.
Causes
No one is sure what causes vulvodynia. But it is known that it is not caused by cancer or certain infections, such as human papillomavirus (HPV) or herpes. It is not a sexually transmitted disease. Once your doctor has diagnosed vulvodynia, he or she has ruled out cancer or herpes.
Vulvodynia may be the result of more than one factor, such as:
- Infections
- Genetic factors
- Spasms of the muscles that support the pelvic organs
- Allergies to certain chemicals or substances
- Hormonal changes, including those that occur with a menstrual cycle or birth control use
- Damage or irritation of the nerves of the vulva
- History of sexual abuse
- Overuse of topical medications
Vulvar pain can be a symptom of many conditions that, once diagnosed, may be treated. For instance, herpes or certain skin diseases can cause vulvar pain, burning, or swelling. However, many times an exact cause for vulvar pain cannot be found. This does not mean that there is no cause, just that one has not yet been found. When no cause is found for vulvar pain, it is called vulvodynia.
Symptoms
Women with vulvodynia may have some of these feelings around vulva:
- Burning
- Stinging
- Rawness
- Itching
- Aching
- Soreness
- Throbbing
- Swelling
These symptoms may be constant, or they may come and go. They can begin and end without any warning. Symptoms also may occur after physical contact with the vulvar area, such as during tampon insertion, sex, or while wearing tight-fitting underwear. Symptoms also may be felt during exercise, after urinating, or even while sitting or
resting.
Diagnosis
To diagnose vulvodynia, the doctor will do a physical exam and tests. He or she may ask questions about:
- Symptoms—what they feel like, how long they last, what brings them on, what makes them feel better, what makes them feel worse
- Lifestyle—diet, exercise, clothing, and any hygiene, skin, deodorant, cosmetic, or laundry products that are used
- Medical history—any recurrent infections or skin problems
- Medications—those currently taken or those taken in the past (including over-the-counter)
The doctor also will examine the vulva and vagina carefully. A sample of discharge from your vagina may be taken and tested for signs of yeast and other infections that could be causing the symptoms.
A swab test also may be performed. For this test, the doctor will use a cotton swab to touch different areas of the vulva and vestibule to find the location and intensity of the pain. He or she will probe the vulva to find areas where the pain is absent, mild, moderate, or severe. If any skin changes are found during the exam, the doctor also may suggest other tests, such as a biopsy or colposcopy.
Treatment
There are many kinds of treatment that may help relieve the symptoms of vulvodynia. No one method works all the time for everyone. Some treatments take a few months before any relief is noticed. Sometimes more than one treatment may be needed. The key is to remain patient and work closely with your doctor. With time, your doctor can help you find the best treatment for you.
Vulvar Hygiene
Gentle care of the vulva can help provide relief from the pain of vulvodynia:
- Wear 100% cotton underwear (no underwear at night)
- Avoid tight-fitting undergarments and pantyhose
- Avoid douching
- Use mild soaps for bathing and clean the vulva with water only
- Do not use vaginal wipes or deodorants or bubble bath
- Do not use pads or tampons with deodorants
- Use lubrication for intercourse
- Apply cool gel packs to the vulva area to reduce pain and itching
- Avoid exercises that put pressure directly on the vulva, like bicycling.
Because different triggers may provoke each woman’s symptoms, pay close attention to what makes yours feel worse. Avoid these items or activities and the symptoms are likely to improve over time.
Medications
Your symptoms may be treated with medications, including:
- Local anesthetics that can provide temporary relief from pain and other symptoms
- Steroids
- Certain types of antidepressants and anti-convulsants
Treatment may relieve symptoms for a while, but they may come back later. Be sure to tell your doctor about medications you are already taking. Some medications have side effects and may make vulvodynia worse.
Other Options
Other things may help you cope with the pain. One of them is to make changes in your diet. Certain foods, like greens, chocolate, berries, beans, and nuts may produce urine that is irritating. They contain chemicals called oxalates. Eating less of these and other highoxalate foods may help.
Some women may try physical therapy or biofeedback. Physical therapy treats muscle spasms and teaches exercises that strengthen the pelvic muscles. Biofeedback trains you to control the muscles in the vagina. Control of these muscles may help lessen your pain. Women with vaginismus also can learn exercises that will help with muscle control during sex.
Since vulvodynia can affect your daily life and relationships, your doctor also may suggest that you receive therapy or sexual counseling. With therapy, a counselor will help you learn to cope with difficult situations. This may help reduce stress and, therefore, the number of painful symptoms. Sexual counseling can provide support for a woman and her partner.
Surgery
For women with severe localized pain who have not found relief through other treatments, surgery may be an option. A vestibulectomy, involving removal of the painful tissue of the vestibule, has been helpful for some women with localized vulvodynia. For these women, vestibulectomy can help relieve pain and improve sexual comfort. It is not recommended for women with generalized vulvodynia.
Finally…
Dealing with the chronic pain of vulvodynia can be hard. Finding the cause of the pain can be frustrating. Although there may be no cure for your condition, you may find some relief with treatment. Your doctor will work with you over time to find a method of treatment that works best for you.
Glossary
Anxiety: A treatable medical disorder characterized by excessive worry, dread, and tension.
Biopsy: A minor surgical procedure to remove a small piece of tissue that is then examined under a microscope in a laboratory.
Colposcopy: Viewing the cervix, vulva, or vagina under magnification with an instrument called a colposcope.
Depression: A treatable medical disorder characterized by loss of interest in things you used to enjoy and feeling sad for periods of at least 2 weeks.
Hormonal: Having to do with hormones, substances produced by the body to control the functions of various organs.
Oxalates: Chemicals found in many foods that can be irritating to people with pain conditions, like vulvodynia, fibromyalgia, and irritable bowel syndrome.
Vaginismus: Involuntary spasm of the pubic muscles and lower vagina that makes penetration by the penis difficult, painful, or impossible.
Vestibulectomy: Surgical removal of painful tissue of the vaginal vestibule.
