Genital herpes is a viral infection that can be spread through sexual contact. It affects one in five adults in the United States—about 45 million people. It is more common in women than in men. This page explains:
- Symptoms of genital herpes
- How to reduce your risk of getting the virus
- How to live with herpes and how to prevent infecting others
What Is Genital Herpes?
Genital herpes is a sexually transmitted disease (STD). It is spread through close contact, most often during sexual activity.
Genital herpes is probably best known for the sores and blisters it causes. These sores can appear around the lips, genitals, or anus. The place where the sores appear is the original site where the virus entered your body. Genital herpes can be spread through direct contact with these sores, but it also can be spread even if you do not see a sore.
Herpes affects millions of people in the United States. Over time, most people with herpes find ways to cope with the disease.
How Infection Occurs
The herpes virus can pass through a break in your skin during vaginal, oral, or anal sex. It can enter the moist membranes of the penis, vagina, urinary opening, cervix, or anus.
Once the virus gets into your body, it infects healthy cells. Your body’s natural defense system then begins to fight the virus. This causes sores, blisters, and swelling.
Besides the sex organs, genital herpes can affect the tongue, mouth, eyes, gums, lips, fingers, and other parts of the body. During oral sex, herpes can be passed from a cold sore around the mouth to a partner’s genitals or vice versa. You even can infect yourself if you touch a sore and then rub or scratch another part of your body, especially your eyes.
The herpes virus can survive for a few hours outside the body. However, there is no proof it can be picked up from toilet seats, hot tubs, or other objects.
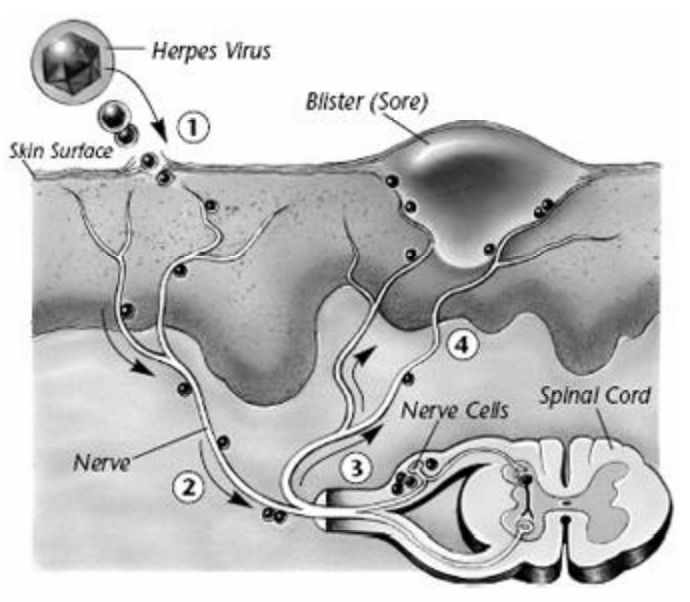
The herpes virus passes through your skin (1). It travels through your body (2) and settles at nerve cells near your spine (3). When something triggers a new bout of herpes, the virus leaves its resting place and travels along the nerve, back to the surface of the skin (4).
Symptoms
Many people infected with herpes have no symptoms. When symptoms do occur, they vary with each person. Some people have painful attacks with many sores. Others have only mild symptoms. If you get symptoms, they usually appear about 2–10 days after the herpes virus enters your body. At this time, you may feel like you have the flu. You may get swollen glands, fever, chills, muscle aches, fatigue, and nausea. You also may get sores. Sores appear as small, fluid–filled blisters on the genitals, buttocks, or other areas. The sores often are grouped in clusters. A stinging or burning feeling when you urinate also is common.
The first bout with genital herpes may last 2–4 weeks. During this time, the lesions break open and “weep.” Over a period of days, the sores become crusted and then heal without leaving scars.
If lesions recur, you may feel burning, itching, or tingling near where the virus first entered your body. You also may feel pain in your lower back, buttocks, thighs, or knees. These symptoms are called a prodrome. A few hours later, sores will appear. In recurrent infections, there is usually no fever and no swelling in the genital area. Sores heal more quickly—within 3–7 days in most cases. Also, recurrent infections usually are less painful.
See your doctor right away if you have symptoms of genital herpes. Similar symptoms may be caused by other infections, so your doctor should confirm the diagnosis.
Diagnosis
Your doctor can diagnose herpes using one or more tests to detect infection. The most accurate way is to obtain a sample from the sore and see if the virus grows in a special fluid. Test results may take about 1 week. A positive result confirms the diagnosis, but a negative result does not rule it out. Blood tests also can be helpful in some cases. These tests check for the antibodies that a woman’s body produces to fight the virus. This can help show if it is a new infection or a recurrent outbreak.
Treatment
There is no cure for genital herpes. There are, however, oral medications to help control the course of the disease. Medication can shorten the length of an outbreak and help reduce discomfort.
If you have repeat outbreaks, taking medication on a daily basis can greatly reduce the symptoms. In many cases, it can prevent outbreaks for a long time. It also reduces the chance that you will give herpes to someone else. Some women choose to take medication just during the time of prodromal symptoms and when the sores appear. Ask your doctor which type of treatment is right for you.
Most people can tell when they are having an outbreak. Learning what to do during an outbreak also can help reduce discomfort that goes with it (see below). Some women have a severe case of herpes. They may need to be treated in a hospital with intravenous medications (medications that are injected directly into a vein).
If You Have a Herpes Outbreak
The following tips may help relieve some discomfort of herpes:
- Keep the lesions clean and dry.
- Use a hair dryer on the low setting to dry sores that are very sensitive or hard to reach.
- Wear loose–fitting cotton underclothes and avoid pantyhose. Nylon and other synthetics hold in heat and moisture, which may slow the healing process.
- Take aspirin or acetaminophen to relieve the pain.
Avoiding Recurrence
Although herpes sores heal in days or weeks, herpes does not leave your body. The virus travels to nerve cells near your spine. It stays there until some event triggers a new bout. The virus then leaves its resting place and travels along the nerves, back to where it first entered the body. This can cause new blisters to occur. Sometimes the virus is present even when you do not see any sores.
No one is sure why some people have recurrences of herpes. One trigger seems to be stress—both emotional and physical. Outbreaks may recur when a woman is under pressure. In other cases, they may recur when a woman’s resistance is lowered by a cold or the flu. To help prevent outbreaks, keep your body strong—get plenty of rest, eat a balanced diet, and learn to cope with stress.
About 90% of people with herpes have repeat outbreaks. How often these outbreaks occur varies greatly from person to person. Some people have only one or two outbreaks a year. Others have as many as five to eight. But, most repeat bouts are milder than the first.
Prevention
If you or your partner have oral or genital herpes, avoid sex from the time of prodromal symptoms until a few days after the scabs have gone away. Not having sex does not mean you cannot kiss, hug, or cuddle. Just be sure that lesions and their secretions do not touch the other person’s skin. Wash your hands with soap and water after any possible contact with lesions. This will keep you from reinfecting yourself or passing the virus to someone else.
It is possible for you to pass herpes to someone else even when you do not have sores. This is because the virus can be present without causing any symptoms. Using a condom may reduce your risk of passing or getting genital herpes, but does not protect against all cases. Although the virus does not cross through the condom, lesions not covered by the condom can cause infection. Using a condom will help protect you from other STDs, though.
Genital Herpes and Pregnancy
If you are pregnant and have herpes, tell your doctor. During pregnancy, there are increased risks to the baby, especially if it is the mother’s first outbreak. Although rare, when a newborn is infected, it most often occurs when he or she passes through the mother’s infected birth canal. A herpes infection can cause serious problems in newborns, such as brain damage or eye problems.
If you are infected with the herpes virus for the first time during pregnancy, there are medications you can take to reduce how severe the symptoms are and how long they last. Women who are infected for the first time in late pregnancy have a high risk (30–60%) of infecting the baby. This is because the woman’s immune system has not yet developed antibodies against the virus. Women who were infected before pregnancy have antibodies against the virus, which also help protect the baby.
If you are infected with herpes and are pregnant, your doctor may give you medication that makes it less likely that you have an outbreak of herpes at or near the time your baby is born.
In some cases, women who have a recurrent bout of genital herpes can take a medication during the last 4 weeks of pregnancy to help reduce the risk of an outbreak at the time of delivery and prevent infection in the baby.
If you have sores or prodromal symptoms at the time of delivery, you will need to have a cesarean delivery. A cesarean delivery may reduce the chance the baby will come in contact with the virus. This is because a cesarean delivery takes place through a surgical cut in the abdomen, where the tissue is not infected with the virus.
Rarely, a baby can be infected without passing through the vagina. This can occur if the amniotic sac has broken a few hours before birth. If a woman does not have sores or prodromal symptoms at the time of delivery, a vaginal birth may be possible.
In most cases, a woman infected with genital herpes can breastfeed without infecting her child. The herpes virus cannot be passed to a baby through breast milk. However, the baby could get infected by touching a blister or sore on the mother’s breast.
If you have sores on your nipple, you should not breastfeed your baby on that breast. Pump or express your milk by hand from that breast until the sore is gone. Be sure the parts of your breast pump that touch the milk do not touch the sore while pumping. If this happens, the milk should be thrown away.
Finally…
Herpes affects millions of people in the United States. It can be a source of concern and discomfort. Simple measures can ease the symptoms of herpes, and medication can promote healing. Over time, most people with herpes find ways to cope with the disease.
Glossary
Amniotic Sac: Fluid–filled sac in the mother’s uterus in which the fetus develops.
Antibodies: Proteins in the blood produced in reaction to foreign substances.
Cesarean Delivery: Delivery of a baby through an incision made in the mother’s abdomen and uterus.
Prodrome: Symptoms that precede the onset of a disease.
Sexually Transmitted Disease (STD): A disease that is spread by sexual contact, including chlamydial infection, gonorrhea, genital warts, herpes, syphilis, and infection with human immunodeficiency virus (HIV, the cause of acquired immunodeficiency syndrome [AIDS]).
Source: acog.org
