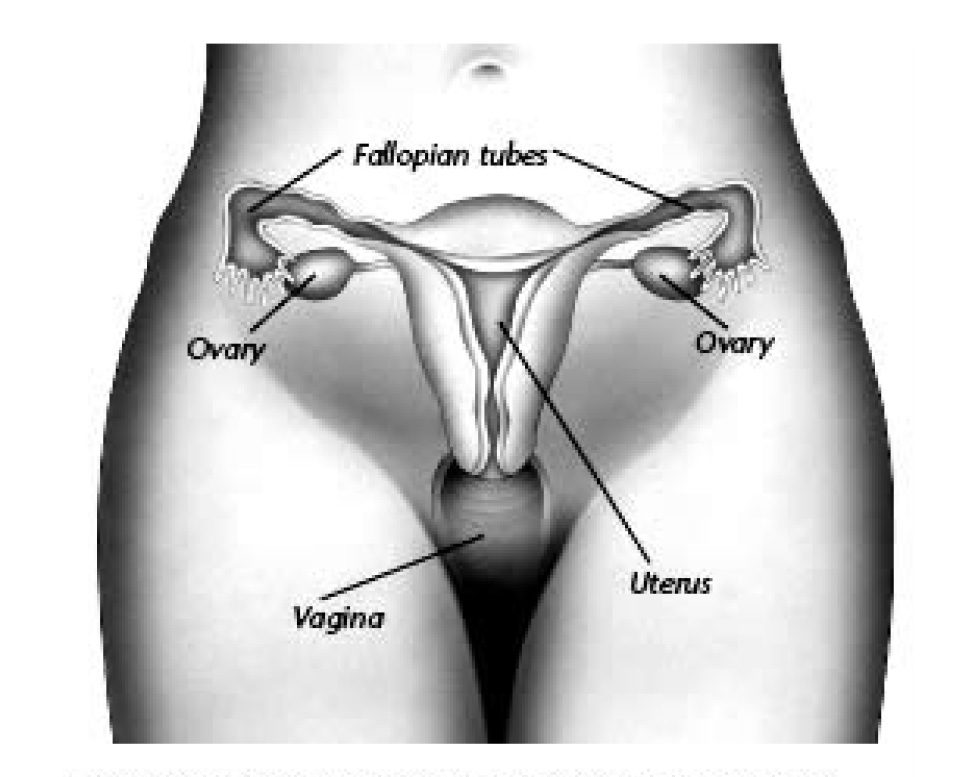
Cancer of the ovary is a disease that affects one or both ovaries, the two organs on either side of the uterus. Ovaries contain eggs that are released when a woman ovulates. They also produce hormones for reproduction. If cancer of the ovary is found and treated early, the cure rate is good. Patients whose cancer has not spread outside the ovary have a 90– 95% chance of living 5 years or longer after treatment.
This page explains:
- Who is at risk of cancer of the ovary
- What are the warning signs
- How cancer of the ovary is detected and treated
Women should be aware of their risk of ovarian cancer. It is important for women to be alert to changes in their bodies and to discuss them with a doctor.
What is Cancer?
Normal, healthy cells throughout a person’s body grow, divide, and are replaced on a routine basis. Sometimes, cells develop abnormally and begin to grow out of control. When this happens, the cells form growths or tumors. Tumors can be benign (not cancer) or malignant (cancer). Benign tumors do not spread, or metastasize, to other body tissues. Malignant tumors can invade and destroy nearby healthy tissues and organs. Cancer cells also can spread to other parts of the body and form new cancerous areas. There are three types of ovarian cancer:
- Epithelial
- Germ cell tumors
- Sex cord–stromal tumors
The type of cancer is based on the type of cells in which it occurs. Epithelial cancers are most common. About 85–90% of all ovarian cancers arise from epithelial cells. These are the cells that cover the surface of the ovaries. Most women who get this type of ovarian cancer are older than 40 years. About 5% of ovarian cancers are germ cell tumors. Germ cells are the cells in the ovary that develop into eggs. Sex cord–stromal tumors occur in connective tissue inside the ovary.
Who is at Risk?
About 3% of all new cancers found in women each year are ovarian cancers. Women of any age can have cancer of the ovary, but the risk increases with age. The most common type occurs most often in women between the ages of 50 and 75 years. Half of all ovarian cancers are found in women older than 63 years. Cancer of the ovary is much less common in women younger than 40 years. It occurs more often in white women than in women of other races.
The fewer times a woman ovulates in her lifetime, the lower her risk of cancer of the ovary. Therefore, women who have had children are less likely to get ovarian cancer because they do not ovulate when they are pregnant or breastfeeding. Women who use birth control pills do not ovulate and thus are less likely to get ovarian cancer. Women who have had tubal sterilization appear to get ovarian cancer less often, but the reason is not clear.
Certain factors can increase a woman’s risk of ovarian cancer:
Family history of ovarian, breast, or colorectal cancer- Personal history of breast cancer
- Late menopause (after age 50 years)
Using fertility drugs also may increase a woman’s risk of this type of cancer. Women who have never been pregnant, or who were pregnant for the first time at age 30 years or older, also have an increased risk.
About 5–10% of all ovarian cancers occur in women who have certain genes (BRCA1 and BRCA2) passed on from their parents. Women with the BRCA1 gene have a 45% lifetime risk of getting the disease. Those with the BRCA2 gene have a 25% risk. Blood tests can tell if a woman carries one of these genes. Women who have one of these genes should see a genetic counselor to learn more about their risk of cancer.
A woman may have some or all of these risk factors and never have ovarian cancer. A woman with no known risk factors can have ovarian cancer. All women should know the symptoms of ovarian cancer and report them to their doctors.
Symptoms
The symptoms of cancer of the ovary often are confused with other health problems. In some cases, there are no symptoms. As a result, ovarian cancer is most often first found in advanced stages (after it has spread). About 20% of ovarian cancers are found in early stages (before it has spread).
Warning signs can include:
- Pain or pressure in the pelvic area or back
- Indigestion, gas, and bloating that cannot be explained
- Abnormal vaginal bleeding
- Pain or swelling of the abdomen
- Increase in abdominal size
- Increased feeling to urinate or changes in bowel habits
- Feeling tired
- Weight loss
Most women with these symptoms do not have a severe problem. They should discuss them with a doctor, though.
Screening
A screening test is a test that is done when there are no symptoms or known risk factors present. There is no good test to screen for cancer of the ovary. For this reason, routine testing for ovarian cancer is not recommended. Your doctor may be able to feel a cyst on one or both ovaries during your annual pelvic exam. Very few of these cysts will prove to be cancer, but they should be checked by your doctor.
The CA 125 antigen may be found in the blood of women with ovarian cancer and may be a sign of the disease. However, other conditions, including fibroids, endometriosis, pelvic infection, pregnancy, and even menstruation, can cause CA 125 levels to be higher than normal. For a very few women, CA 125 levels may be high even though they have no health problems at all. The CA 125 blood test may produce results that suggest that a woman has ovarian cancer when she really does not. This is called a false-positive test result.
Some ovarian cancers do not increase CA 125 levels. In this case, a woman may be told she does not have ovarian cancer when, in fact, she does. This is a false-negative test result.
Normal CA 125 levels are found in about 50% of women with early stage ovarian cancers. About 20–25% of women with advanced ovarian cancers do not have higher CA 125 levels.
The Pap test is a good way to screen for cervical cancer, but it cannot detect ovarian cancer. New tests are being studied to help find ovarian cancers early.
Treatment
If a woman is thought to have ovarian cancer, surgery is needed. It is best that a doctor specially trained or experienced in cancer surgery, such as a gynecologic oncologist, perform this surgery. The surgeon will explore the extent of the disease, remove the cancer, and decide what other treatment is needed.
The disease will be staged as a result of this surgery. Treatment is based on the stage and how fast the cancer is spreading. The age, health, and wishes of the patient also are taken into account when planning the treatment.
Surgery for most patients includes removing the uterus (hysterectomy) and the ovaries and fallopian tubes (salpingo-oophorectomy). Sometimes, some lymph nodes and parts of the bowel may be removed. For women who have early stage cancer of only one ovary and who want to become pregnant, only the ovary with cancer may be removed. The surgery often is followed by chemotherapy. Radiation rarely is given for cancer of the ovary.
If a woman is at very high risk of getting cancer of the ovary (such as those who have the BRCA1 or BRCA2 gene), both fallopian tubes and ovaries may be removed even if she does not have cancer. This is called prophylactic salpingo-oophorectomy. It reduces the chances of getting cancer of the ovary. Once both ovaries are removed a woman cannot become pregnant using her own eggs. She also will go through menopause.
After Treatment
Women treated for cancer of the ovary need to have regular checkups. The doctor may perform a pelvic exam, depending on the extent of surgery. Blood tests to check CA 125 levels will likely be done on a routine basis. Other tests, including ultrasound, chest Xray, or computed tomography, also may be done.
Finally
Women should be aware of their risk of ovarian cancer. It is important for women to be alert to changes in their bodies and to discuss them with a doctor. If you are concerned about cancer of the ovary, talk to your doctor. Your doctor and the other people involved in your health care will do all they can to help.
Glossary
Antigen: A substance, such as an organism causing infection or a protein found on the surface of blood cells, that can induce an immune response and cause the production of an antibody.
BRCA1 and BRCA2: Genes that increase your risk of breast cancer and certain other types of cancer.
Computed Tomography: A type of X-ray procedure that shows internal organs and structures in cross section. Also known as a CT scan or CAT scan.
Endometriosis: A condition in which tissue similar to that normally lining the uterus is found outside of the uterus, usually on the ovaries, fallopian tubes, and other pelvic structures.
Fibroids: Benign growths that form in the muscle of the uterus.
Lymph Nodes: Small glands in the abdomen and other areas of the body that filter the flow of lymph, a nearly colorless fluid that bathes body cells. Lymph can carry abnormal cells to other parts of the body.
Menopause: The process in a woman’s life when ovaries stop functioning and menstruation stops.
Ovulates: Releases an egg from one of the ovaries.
Pap Test: A test in which cells are taken from the cervix and vagina and examined under a microscope.
Prophylactic Salpingo-oophorectomy: Surgical removal of healthy fallopian tubes and ovaries.
Stages: Refers to the size of a tumor and the extent (if any) to which the disease has spread. Stages of ovarian cancer range from I to IV, with I being the earliest and IV the most advanced.
Tubal Sterilization: A method of female sterilization in which the fallopian tubes are closed by tying, banding, clipping, or sealing with electric current.
Source: acog.org
