Sterilization is a permanent method of birth control and a very effective way to prevent pregnancy. It requires a woman or a man to have surgery. The most common sterilization procedure for women is called tubal sterilization. The procedure for men is called vasectomy. In most cases, sterilization is safe and free of problems.
This page will explain:
- Methods of sterilization for both women and men
- Risks and benefits
- Other options for birth control
Making the Decision
Sterilization is an elective procedure. This means you can choose whether to have it done. It should be thought of as lifelong. You must be certain that you do not want children in the future.
Because sterilization is a major decision, you should avoid making this choice during times of stress (such as during a divorce or after losing a pregnancy). You also should not make this choice under pressure from a partner or others. Studies have shown that women younger than 30 years are more likely than older women to regret having the procedure. The procedure can be canceled if you are not sure that permanent sterilization is right for you.
If you are sterilized and you change your mind after the operation, attempts to reverse it may not work. The success of reversal depends on a number of factors (such as type of sterilization, health and age of the person, or length of time since the procedure).
Sterilization is a highly effective and lifelong means of birth control for both women and men. If you have any questions or concerns about having sterilization done, discuss them with your doctor.
After tubal sterilization is reversed, many women are still not able to get pregnant. Also, the risk of problems such as ectopic pregnancy is increased. In men, the chances that a vasectomy can be reversed with success also vary widely. Reversing any sterilization for women or men requires major surgery and expense.
If you are not sure you want to be sterilized, there are a number of short-term methods of birth control:
- Hormonal contraceptives (birth control pills, ring, patch, injections)
- Intrauterine device (IUD)
- Barrier methods:
- Condom (male and female)
- Spermicides (cream, jelly, or foam)
- Diaphragm
- Cervical cap
- Natural family planning and periodic abstinence
Although most birth control methods are not as effective as sterilization, they all protect against pregnancy. If you are sure that you no longer want to be able to have children, you may wish to choose sterilization. However, sterilization does not prevent sexually transmitted diseases (STDs). Condoms should be used for protection against STDs.
If you have doubts about the procedure at any time—even after you have signed papers giving consent—let your doctor know. You can discuss your concerns. If you wish, the operation can be canceled.
Sterilization for Women
All of a woman’s reproductive organs are in her pelvis. The uterus, which is in the lower abdomen, opens into the vagina. A woman has two ovaries, one on each side of the uterus. The ovaries contain eggs. Each month during ovulation an egg is released from the ovary and moves into one of the fallopian tubes. If a woman has sex with a man around this time, an egg may meet a sperm in the fallopian tube and the two may join. This joining is called fertilization. The fertilized egg then moves through the fallopian tube into the uterus and becomes attached there to grow during pregnancy.
In a sterilization procedure, both fallopian tubes are closed by being cut, tied, or sealed. This prevents the egg from moving down the tube and keeps the sperm from reaching the egg.
The Procedure
Tubal sterilization can be done in a number of ways. The methods used most often are laparoscopy, minilaparotomy, and hysteroscopy. Some women may choose sterilization to be done after giving birth. This is called postpartum sterilization. If you are having a cesarean birth, sterilization may be performed at the same time, without the need for additional surgery or a prolonged hospital stay. With all methods, anesthesia (pain relief) is used and you likely can go home the same day. You and your doctor will decide which method is best for you.
Tubal sterilization does not cause your menstrual periods to change. However, if you used birth control pills before you have the surgery, it may take a while to return to your normal cycle. Your periods also may be longer and heavier than when you used birth control pills. This is because birth control pills decrease the amount and length of your period. Tubal sterilization does not affect your ability to have or enjoy sex.
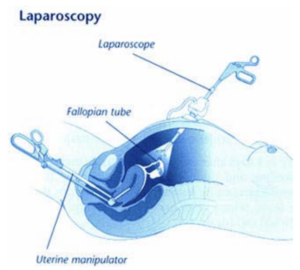
Laparoscopy
Anesthesia is given before the laparoscopic surgery begins. The procedure then follows these steps:
- A small incision (cut) is made in or near the navel.
- A gas (carbon dioxide in most cases) may be passed into the abdomen to inflate it slightly. This moves the abdominal wall away from the organs.
- The laparoscope (a slender, light-transmitting device) is inserted into the abdomen. This allows the doctor to see the pelvic organs.
- A device, called a uterine manipulator, may be placed in the cervix to help move the uterus.
- A smaller device is inserted to move and hold the tubes. The device may be inserted either through the laparoscope or through a second tiny cut made just above the pubic hairline.
- The tubes are sealed by using a ring, clip, or electric current.
- The gas (if any was used) in the abdomen is withdrawn. The cuts are then closed with one or two stitches.
Minilaparotomy
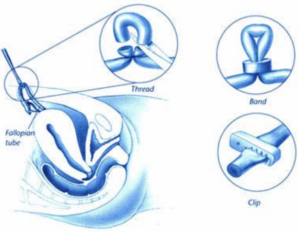
- A small (1-2 inch) cut is made in the abdomen just above the pubic hairline or below the naval.
- The doctor may remove sections of the tubes. He or she will use special thread to tie the new openings shut. Or, the tubes may be closed with electric current (not shown in below image), bands, or clips.
- A few stitches are used to close the cut. It is then covered by a small bandage.
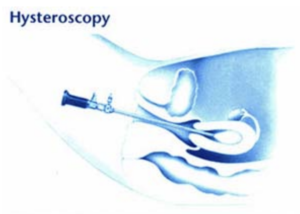
Hysteroscopy
With the hysteroscopic method, a tiny spring-like device is inserted through the vagina into each fallopian tube. This device causes scar tissue to build up in the tubes. This buildup blocks the fallopian tubes and prevents the sperm from reaching the egg.
Afterwards
As with any surgery, sterilization has some risk. Serious complications, such as infections, bowel injuries, bleeding, burns, or complications from anesthesia, are very uncommon. Most of the time, the problems can be treated and corrected.
Side effects after surgery vary and may depend on the type of anesthesia used. You likely will have some pain in your abdomen and feel tired. Other side effects occur less often, including:
- Feeling dizzy
- Feeling sick to your stomach
- Shoulder pain
- Abdominal cramps
- Gassy or bloated feeling
- Sore throat
In most cases, most or all of these symptoms go away within 1–3 days. After that time you may feel tired later in the day, have slight soreness over the cut, and have minor changes in bowel movements. Discomfort can be relieved with pain medication. If discomfort does not go away after a few days or gets worse, call your doctor.
The risk of getting pregnant after tubal sterilization is very low (less than 1%). However, sometimes the sterilization does not work and a woman can get pregnant. In women who have had tubal sterilization and get pregnant, more than half of these pregnancies are ectopic. Call your doctor if you miss a menstrual period after the procedure and think you might be pregnant.
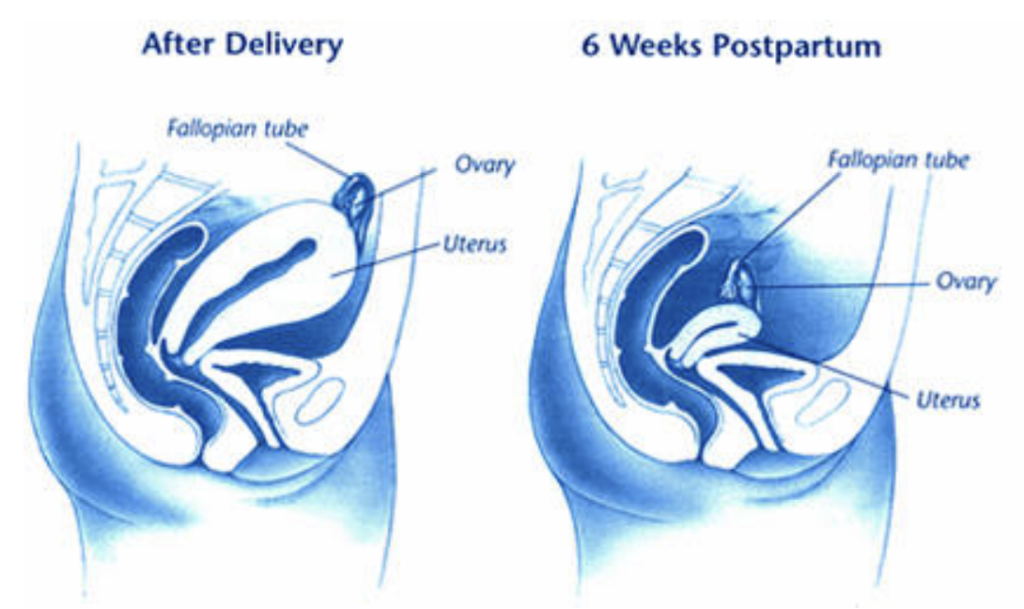
Just after birth, the uterus is still enlarged and the ovaries and fallopian tubes are pushed up just under the surface of the abdomen (left). This gives the doctor easier access to the tubes than he or she would have several weeks after delivery (right).
Sterilization for Men
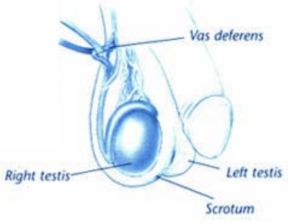
The man provides the sperm that fertilizes the woman’s egg. Sperm are made in the man’s testes. They leave the testes through small tubes called the vas deferens, or vasa. These tubes carry the sperm to a larger tube in the penis called the urethra. As sperm travel through the vasa, they mix with fluid from the seminal vesicles and prostate gland. This mixture of sperm and fluid is called semen. When the man ejaculates (climaxes) during sex, semen travels out through the penis and into the woman’s vagina.
In a vasectomy, the vasa are tied, cut, clipped, or sealed to prevent the release of sperm. This prevents a woman’s egg from being fertilized with the man’s sperm.
The Procedure
A vasectomy may be done in a doctor’s office, clinic, or hospital. The man can go home the same day. The procedure is simple and works very well. There are rarely any serious side effects.
After cleaning the scrotum, the doctor locates each vas in the scrotum. Each side of the scrotum is numbed with pain relief medication. One or two small openings are then made into the skin of the scrotum. Each vas is pulled through the opening until it forms a loop. A small section is cut out of the loop and removed. The two ends are tied and may be sealed with heat. This causes scar tissue to grow to block the tubes. Each vas then is placed back in the scrotum.
Recently, some doctors have begun to use a “no-scalpel” technique for vasectomy. In this procedure, the vas deferens is cut the same way, but instead of making an incision, a special tool is used to puncture the scrotum in one place. No stitches are needed after the procedure. Patients have less pain afterward, and recovery time is shortened.
After the surgery, the man should:
- Rest
- Apply ice packs to the scrotum
- Wear an athletic supporter (“jock strap”)
For 2–3 days after the procedure, there may be some swelling and discomfort in the scrotum. If these symptoms last for more than a few days, or if there is fever, severe pain, or other symptoms, the man should call his doctor.
Afterwards
Unlike tubal sterilization in women, a vasectomy is not effective right away. Some sperm still may be in the tubes. For this reason, a couple must use another method of birth control until a return visit to the doctor or clinic for a final sperm count (in which the number of sperm in a semen sample are counted). It takes about 1–3 months for the semen to become totally free of sperm.
After a vasectomy, a man’s sexual function does not change. A man can have sex again as soon as he feels ready. He can have an erection and ejaculate (climax) normally. Because sperm normally make up only 5% of semen, there will be little change in the amount of fluid that is released.
Vasectomy is highly effective—less than 1% of vasectomies fail to prevent pregnancy. The most common cause of failure is unprotected sex too soon after the procedure. Vasectomy should be thought of as lifelong. As with sterilization of women, vasectomy does not protect against STDs.
Factors That Affect Choice
The method of sterilization a man or a woman chooses will depend on:
- Personal choice
- Physical factors, such as weight
- Medical history
Sometimes previous surgery, obesity, or other conditions may affect which method can be used. The person should be fully aware of the risks, benefits, and other options before making a choice. In most cases, for you and your partner vasectomy has less risk than tubal sterilization of a woman.
Check with your doctor about the timing of sterilization. There may be waiting periods after consent forms are signed. There may be certain age requirements. Discuss the rules and laws that apply in your case with your doctor before surgery. Also, you may want to check if your health insurance covers sterilization procedures.
Finally…
Sterilization is a highly effective and lifelong means of birth control for both women and men. If you have any questions or concerns about having sterilization done, discuss them with your doctor. All of your questions should be answered before the operation.
Glossary
Ectopic Pregnancy: A pregnancy in which the fertilized egg begins to grow in a place other than inside the uterus, usually in the fallopian tubes.
Hysteroscopy: A surgical procedure in which a slender, light-transmitting telescope, the hysteroscope, is used to view the inside of the uterus or perform surgery.
Laparoscopy: A surgical procedure in which a slender, light-transmitting instrument, the laparoscope, is used to view the pelvic organs or perform surgery.
Minilaparotomy: A small abdominal incision used for a sterilization procedure in which the fallopian tubes are closed off.
Sexually Transmitted Diseases (STDs): Diseases that are spread by sexual contact, such as herpes, gonorrhea, and human immunodeficiency virus (HIV, the cause of acquired immunodeficiency syndrome [AIDS]).
Tubal Sterilization: A method of female sterilization in which the fallopian tubes are closed by tying, banding, clipping, or sealing with electric current.
Vasectomy: A method of male sterilization in which a portion of the vas deferens is removed.
