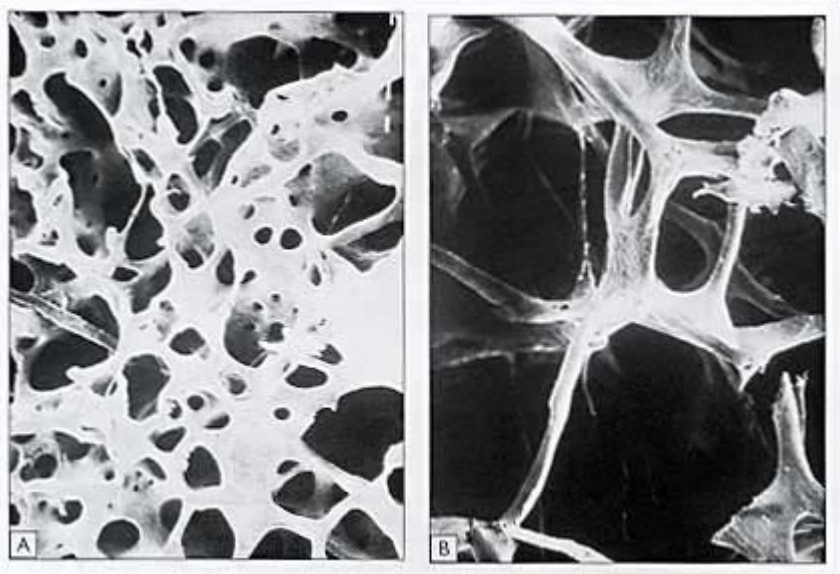
Osteoporosis is the loss of bone density and strength. A normal skeleton is made up of two major types of bone. One type, called cortical bone, is the dense, stiff bone that is the major component of the long bones of the legs and arms and other sites. Another type of bone, called trabecular bone (or “spongy” bone), occurs in areas such as the spine, hips, heels, and wrists, where flexibility and shock absorption are required. Trabecular bone contains many small holes (pores) through which blood circulates. Within these small pores, special cells called osteoclasts break down bone, and other special cells called osteoblasts build bone back up.
The constant process of breakdown and re-formation is called remodeling. One cycle of remodeling takes up to six months. In fact, your entire skeleton is slowly replaced by remodeling every four to five years. Osteoporosis happens when osteoclasts break down bone more quickly than the osteoblasts form new bone. When this happens, your bones will lose strength and density. Trabecular bone loses density more readily than cortical bone.
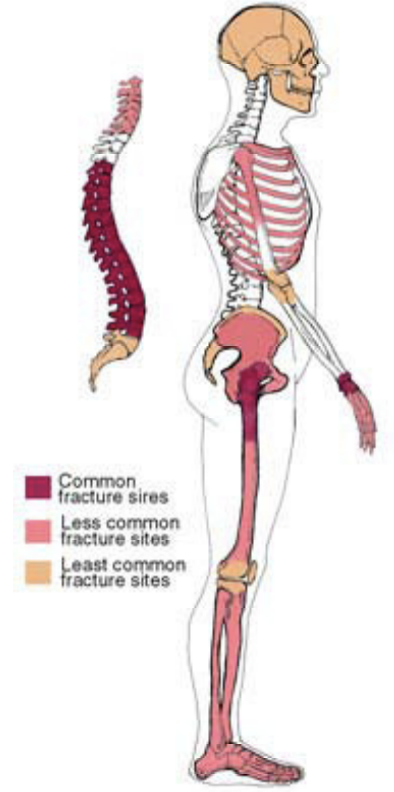
Early bone loss is just thinning of the bone around the already porous areas (osteopenia). At this early stage, bone loss may be fully reversible. If the process of bone loss is not reversed, however, it may eventually lead to severe osteoporosis. Osteoporotic bone contains much larger holes connected only by thin strips of weakened bone. This weakened bone is less dense, and is much more prone to fractures. Sites containing more spongy (trabecular) bone tend to fracture first, which is why hip, spine, and wrist fractures are more common than fractures at other sites. People with more severe osteoporosis have a greater risk of fracturing the ribs and the long bones of the arms and
legs.
Causes
As you age, your bones break down faster than they can build back up. The primary cause of osteoporosis is increasing age. Most women reach their maximum bone density by the age of 35—most men reach their maximum bone density by age 40. After you reach your peak bone density, your bone mass is maintained by a process whereby cells break down and re-form bone (remodeling). As you get older, however, your bones break down more quickly than they re-form. Therefore, your bones become thinner and more likely to break. Age-related losses of balance and muscle strength also increase your risk of falling and breaking a bone.
Poor nutrition and lack of physical activity contribute to decreased bone density. It is important to consume calcium and vitamin D during adolescence and young adulthood. During this time your bones are still building mass, and calcium and vitamin D help to make them as strong as possible. It is also important to get regular physical exercise during this time; especially weight-bearing exercise.
A poor diet and a sedentary lifestyle can hinder bone-building and contribute to brittle bones in later age. Drinking caffeine and soda on a regular basis, in particular, is thought to increase the rate of calcium loss from bones. This is particularly disturbing since many young people now drink soda and coffee instead of milk.
It remains important to get exercise and consume calcium and vitamin D as you age to slow bone loss.
Symptoms
Osteoporosis can occur without any symptoms. You may not realize that your bones are becoming brittle until you get a fracture. Even regular x-rays cannot detect osteoporosis until you have lost more than 20% of your bone density.
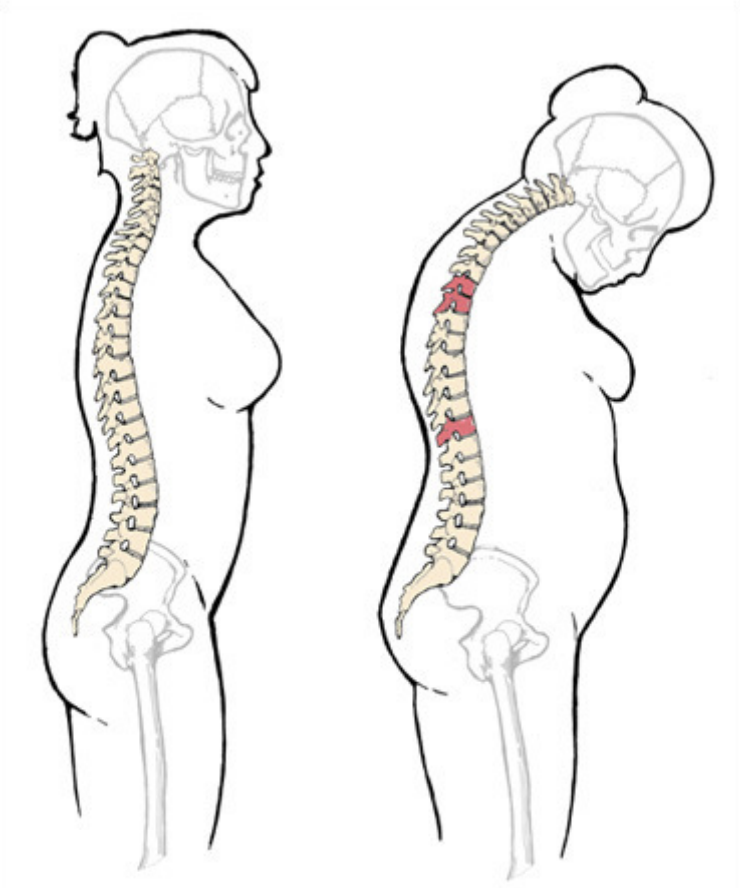
There are, however, some late signs of osteoporosis. A collapsed bone in your back (vertebra), for example, may cause severe back pain, loss of height, or a stooped posture (kyphosis). If you have lost more than 1 ½ inches of height since the age of 35, you are at increased risk for osteoporosis.
A collapsed bone in your back may cause severe back pain, loss of height, or a stooped posture (kyphosis)
Risk Factors
Women are at a greater risk for osteoporosis than men. One out of two women and one out of eight men will break a bone because of osteoporosis after the age of 50. Women have a greater risk of osteoporosis because they have bones that are smaller and less dense than those of men. In addition, women tend to participate in fewer weight bearing activities, and also tend to lose more bone mass than men. Women who have irregular menstrual cycles or no menstrual periods (amenorrhea) and women who have gone through menopause have a greater risk of osteoporosis. During the years just before and after menopause, women can lose about 20% of their bone mass.
Low estrogen levels contribute to brittle bones. Estrogen helps prevent bone breakdown, but doesn’t build bone. Therefore, if you have low estrogen levels, you may experience bone loss that is not replaced, even if your estrogen levels return to normal. Estrogen related bone loss usually tends to occur earliest in the spine, with the hip and wrist losing bone somewhat later on.
Some female athletes stop having their periods (amenorrhea) because the physical exertion changes their levels of reproductive hormones. These women are at risk for osteoporosis because their lack of estrogen causes them to lose bone mass. They may experience stress fractures that are very difficult to treat. This risk does not decrease if they exercise less or take calcium supplements.
Osteoporosis isn’t just a disease of the very old. Some women may lose half their bone mass by age 65 because of prematurely low estrogen levels.
Young women with eating disorders (such as anorexia nervosa) are at risk for dramatic bone loss and stress fractures.
If you are close to or have reached menopause, you are at an increased risk for having osteoporosis. During the time around menopause, some women lose bone as they begin to skip periods and have other menopausal symptoms. Some may have as much as 50% bone loss during the five to seven years before their periods stop and true menopause begins. Women who have reached menopause are at a particular risk for osteoporosis as their estrogen levels further decline.
If you are a woman who has had her uterus removed (hysterectomy), you have a greater risk of osteoporosis.
A total hysterectomy at any age results in rapid bone loss. Even when both ovaries remain following a partial hysterectomy, there is usually a significant decline in estrogen production following removal of the uterus that results in menopause and increased bone loss in about five to eight years.
Osteoporosis from hormone loss also happens to men. Men who have low testosterone levels have a much higher risk for osteoporosis than other men. Osteoporosis related to low testosterone levels has a similar pattern to osteoporosis in women, and can cause significant bone loss in the spine and hip. Low testosterone levels can occur in men at any age; a decrease in sexual function and hair loss are the most common symptoms. All men over the age of 60 experience a decline in testosterone levels. Men who are treated for prostate cancer have a particularly high risk of osteoporosis.
Of the men who have osteoporosis, 20% have a type known as “idiopathic”, a type that has no cause. Idiopathic osteoporosis can occur at any age. As a result, men who have major fractures or fractures with very little trauma, or who have curvature of the upper spine (kyphosis) or unexplained height loss should be screened for osteoporosis.
Insufficient vitamin D intake increases your risk of osteoporosis and decreases response to any osteoporosis treatment plan. Adequate levels of vitamin D are required in order to absorb calcium and to build bone. It is estimated that more than 70% of the population in the northern half of the US are Vitamin D–deficient. This significant bone loss is directly related to inadequate levels of vitamin D and sun exposure. This is true for all age groups, but is even more severe in the elderly. In addition, after age 50, there is a progressive decline in the absorption, metabolism, and effectiveness of vitamin D in both men and women. After about age 50 it is essentially impossible to get enough vitamin D from sun exposure alone. Vitamin D is not readily available in the diet, so supplements are usually required.
Insufficient calcium intake increases your risk of osteoporosis and decreases your response to any osteoporosis treatment plan. Calcium is required to build and maintain bone density at all ages. After the age of about 50, your ability to absorb calcium decreases, which is often made worse if you don’t get enough vitamin D. As a result, you should increase your intake of calcium after age 50. However, you should take your calcium in several smaller doses to optimize absorption.
Having a small-boned frame or being tall increases your risk for osteoporosis. There is a direct relationship between increased height combined with low body weight and osteoporosis in both men and women. In women, body weight of less than 128 lbs has been shown to significantly increase risk of osteoporosis. Low body mass index (BMI) in men or women dramatically increases osteoporosis and fracture risk, as well as increasing risk of falls. In addition, small—boned women have an increased risk of fracture irrespective of bone density due to the decrease in bone mass.
Having either a parent or sibling who has had osteoporosis, a spine or hip fracture, or another fragility fracture increases your risk of getting osteoporosis.
Smoking, drinking alcohol to excess, or leading an inactive lifestyle puts you at risk for osteoporosis. These modifiable risk factors are often major contributors to early osteoporosis in both men and women. In women, tobacco use causes menopause three years earlier than it would occur in a nonsmoking woman. In both men and women, tobacco inhibits normal bone metabolism. Alcohol abuse is a major contributor to osteoporosis (especially in men) because it results in abnormal bone metabolism and is associated with malnutrition. In addition, alcohol abuse carries with it an increased risk of injury and falls, which is dangerous for a person with weakened bones.
Some ethnic groups are more at risk than others. Although risk is higher among Caucasian and Asian women, African-Americans as well as Hispanic-Americans are also at risk for osteoporosis. Among African-American women, for example, 10% over the age of 50 have osteoporosis, and another 30% have low bone density.
Risk Factors for Osteoporosis
Things You Can’t Change
- Age (women: over 50; men: over 60)
- Female gender
- Being tall, having a small frame, or a slender build (weight under 128 lbs or BMI below average)
- Family history (mother, father, or sibling)
- Race (Caucasian or Asian ancestry at greater risk than others)
- Menopause
- Certain diseases (see below)
- History of previous fracture, especially after age 50
- Confusion or dementia and/or unsteady gait and frequent falls that cannot be reversed with treatment
Thing You Can Change
- Stop Smoking
- Drink no more than 2 alcoholic drinks per day, and no more than 6 drinks per week
- Get enough exercise, but not so much as to induce amenorrhea (women)
- Get adequate calcium and vitamin D
- Avoid certain medications (see below)
Drugs that Increase Your Risk for Osteoporosis
Certain drugs increase your risk for osteoporosis by decreasing calcium absorption and vitamin D metabolism, and/or by directly affecting bone formation and breakdown.
Major Culprits
- Corticosteroids at all ages, and also inhaled corticosteroids in the elderly (Prednisone, Medrol, etc.)
- Phenytoin (Dilantin), Phenobarbitol (possibly other, newer anticonvulsants as well)
- Aluminum—containing antiacids (not the more common magnesium containing ones)
- Warfarin (Coumadin), Heparin
- Excessive thyroid hormone replacement (often taken to shrink a thyroid mass)
- Benzodiazipines (Valium, etc)
- Any treatment for prostate cancer.
- Most (possibly all) chemotherapy agents (including interferon, etc.)
- Methotrexate (possibly other, newer rheumatoid arthritis drugs as well)
Other drugs/medications also associated with decreased bone density Insulin
- More than five years of continuous tetracycline use or excess vitamin A or use of oral vitamin A derivatives for acne treatment.
- Gonadatropin—releasing hormone treatment for endometriosis
- Caffeine (also contained in many headache medications)
- Certain diuretic medications (“loop diuretics” such as Lasix, Demidex, Bumex)
- Cholestyramine use for more than five years (used to lower cholesterol)
Diseases Associated with Decreased Bone Density
Some diseases increase your risk of osteoporosis by affecting bone metabolism.
- Overactive parathyroid glands
- Overactive thyroid gland
- Inflammatory bowel disease (Crohn’s or other colitis; not irritable bowel)
- Severe chronic lung disease (emphysema, pulmonary fibrosis, etc.)
- Intestinal sprue, surgery to remove part of the stomach or small intestine, or other causes of malabsorption in the upper intestinal tract
- Cystic fibrosis
- Renal tubular acidosis or chronic renal dialysis
- Chronic immunosupression for any type of organ transplantation
- Osteogenesis imperfecta
- Insulin—dependent (type 1) diabetes
- Cushing’s disease
- Grand mal seizure disorder
- Rheumatoid arthritis (not osteoarthritis)
- Dementia of any type
- Any disease resulting in muscle weakness or paralysis
- History of any previous fracture, especially after age 50
- Dramatic increase in fracture risk with history fracture of either the spine or hip
- Scoliosis
Factors that Increase Bone Mass
There are some factors that have been shown to result in increased bone mass.
- Morbid obesity (weight over 250 lbs or significantly elevated BMI) without increased risk of falls
- Delayed menopause and/or continuous hormone replacement therapy
- More than three pregnancies combined with adequate calcium and vitamin D intake
- Lifetime high intake of milk products (average three or more servings per day)
- Use of Thiazide diuretics for more than five years (decreases calcium excretion)
- Use of “statin” lipid—lowering medications (Zocor or Pravachol or Mevacor) for more than three years
- Lifetime history of extremely heavy weight—bearing activity (involving regular, continuous lifting of more than 40 lbs)
Diagnosis
Your doctor will perform a complete physical exam, and will review your medical history when diagnosing osteoporosis. Diagnosis can be elusive among people with brittle bone disease, mainly because its symptoms are silent. Your doctor should go over your medical history, including your family history, and give you a full physical exam that includes your height, weight, x-rays, and blood and urine samples.
Your doctor may run tests to determine bone density and fracture risk. Anyone who has significant risk factors for osteoporosis, especially older women, should undergo bone density tests. These tests measure bone density in different areas of the body; specifically the hips, wrists, and vertebrae, where osteoporos is related fractures may appear. Such tests can detect osteoporosis before a fracture occurs, and can assess your odds of sustaining a fracture. Also, frequent testing may help to determine your rate of bone loss through the years.
There are different types of tests to measure bone density.
Dual energy x-ray absorptiometry of the hip and spine (DEXA) testing measures bone density of the spine, hip, or total body (when necessary, this method may also be used to measure bone density in the wrist). At present, DEXA of the hip and spine is the preferred test for diagnosis and monitoring of osteoporosis because it is the most precise and reproducible. It is also the only test readily available that can accurately measure bone density in the hip, which is one of the most important diagnostic sites. DEXA tests usually take no more than 10 minutes, and give off much less x-ray irradiation than a mammogram. This test is recommended by most experts as the only dependable diagnostic method for women under age 50, or for men of any age.
CT bone density testing of the spine is used less commonly due to the high x-ray exposure and the inability to measure bone density in any other site than the spine. This test may be used if there are no other options available to you.
Peripheral dual x-ray absorptiometry (DXA) measures bone density of the wrist, heel, or finger. However, this test may miss osteoporosis that has started in the spine and is not yet evident in the extremities (osteoporosis often begins in the spine in women, sometimes years before it is evident in other sites). Peripheral bone density tests have been shown to miss osteoporosis in up to 30% of cases in women younger than 65 years of age.
Ultrasound bone density testing is the most recent diagnostic method approved by the U.S. Food and Drug Administration. This method assesses the risk of osteoporosis in one minute, and uses no x-rays. Bone density is determined by measuring the absorption of high-frequency sound waves by the bone in the heel of your foot. By placing your foot into the device, which is shaped like a box, a picture of the heel bone is taken. The sonometer is less costly than other tests, and may serve as a preliminary screening tool for some high-risk populations, or for
those who cannot have a DEXA scan. In women over 65 years old this test is fairly specific for osteoporosis, but still may miss up to 20% of cases that would be found on DEXA. In men or younger women, however, there can be a very high false negative rate.
Prevention and Screening
To prevent osteoporosis, it is critical to take steps to maximize bone growth in childhood and young adulthood. After your bones reach their peak density, it is equally important to take further preventive measures to avoid the gradual loss of bone that can result in low bone density and osteoporosis later in life.
Maintain healthy eating habits and levels of activity throughout life. Because peak bone mass continues to develop from childhood on through adolescence, parents should pay close attention to the eating and lifestyle habits of their children. Parents should continue to set examples and encourage good eating and lifestyle habits as their children grow to become teenagers and young adults. It is most important to eat a balanced diet with plenty of calcium and vitamin D each day. You should not smoke, and you should limit your intake of soda and caffeine. Other key lifestyle routines that help build stronger bones include doing weight—bearing activities such as lifting weights and walking.
Young women in competitive sports (especially swimming or track) should be monitored closely for normal menstrual cycles, and a physician should evaluate any significant changes. Young women should also be monitored closely for signs of eating disorders, as these have become more and more frequent and can result in significant bone loss.
A bone density test helps to determine your chances of a future fracture. Anyone with significant risk factors for osteoporosis or fracture should consider bone density testing, as treatment can result in major decreases in future fracture risk.
Urgent Care
Call your doctor immediately if you have sudden back pain or a broken bone.
It is especially important to get immediate treatment for a hip fracture. Patients with significant osteoporosis may have major fractures with little or no trauma. Hip fractures are especially critical; 20% of patients over the age of 50 die during the year of their fracture; men have a 26% higher death rate than women within a year of fracturing a hip. These fractures are often debilitating, and can require long-term care. A woman’s risk of developing a hip fracture is equal to her risks of developing breast, uterine, and ovarian cancer combined.
Self Care
Eat a calcium-rich diet to build strong bones. If you find it hard to get the daily recommended amount of calcium, you should take calcium supplements. Eat a balanced diet with plenty of calcium. Foods rich in calcium include: dairy products such as milk, yogurt, and cheese; calcium-fortified foods such as orange juice, bread, and cereals; canned fish with edible bones such as sardines and salmon; leafy dark green vegetables such as kale, collard greens, spinach, and broccoli. Before the age of 40, you should get about 1,000 mg of calcium a day. If you are a woman past menopause, you should consider increasing your daily intake to 1,500 mg of calcium a day (one cup of low—fat milk contains 300 mg of calcium). After about age 40 or 50, you should take calcium supplements in divided doses of not more than 500 to 600 mg per dose. Milk and milk products remain the safest and most effective source of calcium.
Calcium supplements can be found in different forms; calcium carbonate and calcium citrate are both acceptable. Calcium carbonate should always be taken with food to improve absorption. Calcium citrate can be taken at any time, with or without food. Some patients find calcium citrate to be less constipating.
Although there has been a lot of concern over lead contamination in calcium supplements in the past, several recent studies have shown that there is little to no significant lead contamination in the major calcium supplements.
In addition, there is no increased risk for kidney stones from increasing calcium intake as long as it is combined with an adequate intake of vitamin D. Anyone with a history of kidney stones should maximize fluid intake to at least three to four quarts of water a day.
Make sure you get enough vitamin D, as your body needs it to absorb calcium. Your body can’t readily absorb calcium without sufficient amounts of vitamin D. Vitamin D is also required for proper bone metabolism. Spending time outdoors, even for ten minutes each day, will help you get the vitamin D you need, but may still be insufficient. If you live in the northern half of the US (or further north), you are unlikely to be able to get enough vitamin D to help you maximize your peak bone density, or adequately suppress bone loss with age. Dairy products can be a good source for vitamin D if you consume three or more servings each day. You may wish to consider supplementation with 400 U (units) of vitamin D per day from childhood through age 40 (particularly in the winter); especially if your dairy intake is limited. After about age 40 or 50 you should consider increasing your vitamin D intake to 600 to 800 U per day as the production and effectiveness of vitamin D declines with age. If you are being treated for low bone density, you should consider taking 800 U per day of vitamin D supplementation unless other major sources of vitamin D are available. Many calcium supplements come with vitamin D, usually at a dose of 125 to 200 U per pill. Some fortified foods, such as cereals and breads, contain limited amounts of vitamin D.
To ensure your safety, you should always discuss vitamin intake with your clinician– especially if you have a history of chronic diseases or organ problems (liver or kidney, etc), or if you are on any prescription medications.
Fluoride may be useful for maintaining bone. Fluoride is known to fight cavities, and has been postulated to help build bone. However, studies show that the new bone stimulated by large amounts of fluoride intake is weak and abnormal, and is prone to increased fracture risk. The relatively tiny amounts of fluoride typically found in water, toothpaste, or other sources do not seem to have any significant positive or negative effect on bone.
Supplements Used to Prevent Osteoporosis
Calcium Supplements
Calcium, Carbonate, calcium citrate
| Dosing | Special Considerations |
|---|---|
| Premenopausal women and men who have normal bone density: 1,000 mg a day | Calcium carbonate: Always take with food. May cause constipation. |
| Men over age 60 who have normal bone density: 1,200 mg a day | Calcium citrate: May take with or without food. May cause dyspepsia if taken alone (rare). May help constipation. |
| Postmenopausal women and anyone with a low bone density: 1,500 mg a day | Always divide doses greater than 500 to 600 mg. Best taken after noon; avoid taking with caffeine or soda |
| Elderly: 1.2 g per day |
Vitamin D Supplements
| Dosing | Special Considerations |
|---|---|
| Vitamin D 400-800 U per day | Side effects are rare |
Both calcium and vitamin D supplementation can result in kidney stones or symptoms related to high calcium levels (for example, constipation, loss of appetite, or nausea) in elderly patients with underlying or undiagnosed metabolic disease, or in patients with severe osteoporosis if not taken with appropriate medications to suppress bone reabsorption.
Weight-bearing exercises build stronger bones. When your legs, arms, and other parts of the body meet resistance, you build bone. Weight-bearing exercises include weight lifting, gentle running, walking, stair-climbing, and gardening. Swimming and bicycling are not, even though they have benefits for aerobic and cardiac fitness. If done regularly, weight-bearing exercises help to prevent osteoporosis. These types of exercises also help to improve balance, decreasing the chance of a fall. If you have bone loss, you will need to choose exercises that not only help build bone, but are also safe and unlikely to result in falls.
Standing from a chair without pushing off is a simple exercise that can be repeated in sets of five. This exercise has been shown to help decrease bone loss and also improve balance in the elderly.
Exercises that strengthen the back will help to prevent or treat osteoporosis. Exercises that strengthen the back help you maintain or improve posture. A strong back and good posture will help you avoid fractures. Weight—lifting programs using relatively light weights (2-10 lbs) can result in less upper back pain, and, when carefully supervised, can greatly facilitate response to any osteoporosis treatment plan. Weight lifting beyond 10 lbs should be considered only with careful supervision to avoid the increased risk of injury associated with heavier weights. Rowing machines may also be useful in a back strengthening program, although their direct effect on bone density has not been studied. If you smoke, quit. Smoking lowers estrogen levels; smokers have been found to reach menopause more than three years earlier than non-smokers.
Smoking significantly decreases response to hormone-replacement therapy, while also increasing the risks of serious side effects such as blood clots or heart attacks. In addition, smoking may impede calcium absorption, and also impedes the formation of collagen that forms the protein structure of bone and skin.
Consuming excessive alcohol has multiple negative effects on bone density and fracture risk. People who drink excessively (more than 2 drinks in 24 hours and/or more than 6 drinks per week) often suffer from poor nutrition, resulting in bone loss as well as an increased risk of falls and injuries when intoxicated. Studies have shown a major
correlation between alcoholism and osteoporosis in men.
Drug Therapy
Your doctor is the best source of information on the drug treatment choices available to you.
Other Therapies
Practice the Chinese martial art of tai chi to improve balance and prevent a fall. If you have osteoporosis, avoiding a fall is important. About 33% of people over the age of 65 experience a fall. Broken bones at this age can mean long-term rehabilitation or even death. Although there are no scientific studies to prove it, practicing the ancient Chinese martial art of tai chi may be beneficial. The exercise uses slow, flowing movements that increase flexibility and strength, and improve balance. Studies have shown that 30 minutes of daily of practice significantly improves balance.
If you do suffer a broken bone, you may need physical therapy. To recover from a broken bone such as the hip, wrist, or spine, you may need to see a physical therapist. He or she can help devise a therapy plan to fit your degree of bone loss. Talk to your clinician for referrals.
Wearing hip protectors may prevent a fracture if you fall. Hip protectors are hand-sized cups that fit into a special pair of underwear. The hip protector sits over the hip bone, and is held in place by pockets in the underwear. If worn consistently, hip protectors can prevent a hip fracture due to a fall. Hip protectors are available over the internet, or
through medical supply stores.
Surgery
Although still not widely available, a specialized therapy called kyphoplasty may immediately relieve pain and prevent debilitating deformities caused by collapsed vertebrae. Kyphoplasty is an invasive procedure that involves expanding the collapsed vertebrae using “balloons” and injecting “bone-like” material into the crushed vertebrae. The material hardens, and the entire process brings the vertebrae back up to near its original shape. Most patients who have undergone kyphoplasty have immediate relief from most of the fracture-related pain.
Alternative Medicine
Some people use soy and other plants to increase their bone density. However, no studies have confirmed that these substances have a significant effect on bone density. Although soy and other plants contain significant amounts of estrogen-like plant substances (phytoestrogens), there have been no studies to confirm that any substances have a significant effect on increasing bone density. The activity of phytoestrogens is thought to be 20 to 50 times less than the most common human estrogen, estradiol. However, soy and other plants that contain phytoestrogens often do contain calcium and protein, and are generally a good source of nutrition for patients with osteoporois. It remains to be proven if a high daily intake can help prevent osteoporosis.
Talk to your clinician about matters that affect your gait and balance. Bad vision, poor balance, chronic diseases that impair your mental or physical performance and certain medications (such as sedatives) can all lead to a fall. If you are on any of the following medications, you should talk to your clinician about the use of these medications and other concerns that may affect your balance and the way you walk:
- Amitriptyline or Nortriptyline
- Benzodiazipines such as Valium, Xanax, or Ativan
- Over-the-counter medications containing Benadryl
- Sleep medications such as Ambien
Avoid a fall by practicing safe living habits. Take precautions while outdoors to prevent a fall: try using a four—pronged cane for stability; use rubber soled shoes or strap-on treads for traction, avoid slippery sidewalks or carry salt in your pocket to spread onto walkways, and avoid wet polished floors. While indoors, use carpet runners, keep your floors clutter-free, remove loose wires, and do not walk in socks, slippers, or hose. Be sure lighting is adequate and light switches are accessible. Area rugs should be tacked to the floor or have slip-proof backing; make sure stairs have handrails; make sure bathrooms have handrails in the shower, tub, and near the toilet; use a rubber bath mat; only use wide step stools with handrails; keep a cordless phone with you to avoid rushing to answer it; keep a flashlight and batteries at your bedside and consider automatic dial emergency services.
Safe Living Habits to Prevent a Fall
While Outdoors
- Use a four-pronged cane for stability
- Wear rubber-soled shoes or strap on treads for traction
- Avoid slippery sidewalks or carry salt in your pocket to spread on walkways
While Indoors
- Use carpet runner
- Keep floors clutter-free
- Remove loose wire
- Tack area rugs to the floor or use slip-proof backing
- Do not walk in socks, slippers, or hose
- Avoid wet polished floors
- Make sure the stairs have handrails
- Make sure bathrooms have handrails in the shower, tub, and near the toilet
- Use a rubber bath mat
- Only use wide step stools with handrail
- Keep a cordless phone with you to avoid rushing to answer it
- Keep a flashlight and batteries at your bedside
- Make sure your house is well-lit and that light switches are easy to access
Prognosis
Osteoporosis can be life-threatening. Women who fracture a hip have a 20% risk of death in the first year after the fracture. Men have a 33% chance of death in the first year after hip fracture. If you survive a hip fracture, you will still need to make major lifestyle changes. For example, you may not be as independent as you had previously been, or you may even need long—term care.
While there is no cure for osteoporosis, it can be treated. To manage your osteoporosis, it’s important to take preventive measures such as consuming plenty of calcium and vitamin D, doing weight-bearing exercises, and avoiding excessive alcohol and smoking. These same measures can also increase your response to any medication treatment plan by more than 20%. Osteoporosis can also be treated, and may even be avoided or delayed by adequate drug therapy. Extensive studies of the quality of bone formed with osteoporosis have suggested that this bone is identical to younger bone in structure and response to stress.
Follow-Up
Return to your doctor for regular bone density tests. Your doctor can monitor your rate of bone loss, and thus head off low bone density with drug therapy and supplements. It’s never too late; a bone density test is also recommended for older woman who can benefit from different therapies. The tests measure bone density in various parts of the body, and can detect osteoporosis before a fracture occurs. If done regularly once a year, the DEXA bone density test can monitor the results of your treatment. There are also several urine and serum tests that can detect your rate of bone turnover. These tests may also be used to evaluate early treatment response (4 months).
Source: PDR.net
