Pain during sexual intercourse is called dyspareunia. Pain that occurs during other sexual activities is called noncoital sexual pain disorder. Pain during intercourse is very common—nearly 3 out of 4 women have pain during intercourse at some time during their lives. For some women, the pain is only a temporary problem; for others, it is a long-term problem. Painful intercourse has many possible causes. Successful treatment depends on finding the right cause and sometimes trying different treatment options.
This page explains:
- Female pelvic anatomy
- How sexual response problems and gynecologic problems may cause pain during sex
- How your health care provider can help
Understanding Your Body
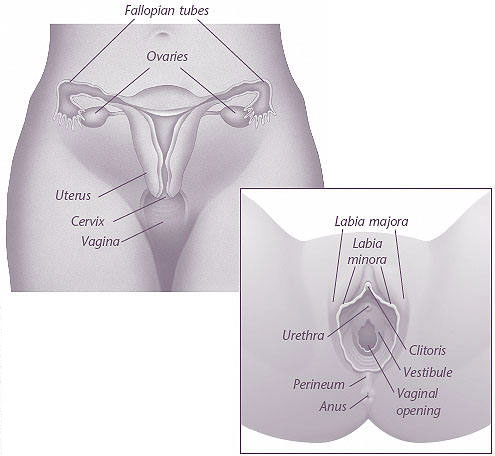
To understand what causes painful sex, it first helps to know about female anatomy so that you can describe the exact location of the pain. You may feel pain in your vulva, in the area surrounding the opening of your vagina (called the vestibule), or within your vagina. The perineum is a common site of pain during sex. You also may feel pain in your lower back, pelvic region, uterus, or bladder.
Sexual Response Problems
Lack of desire, arousal, or both can lead to painful intercourse in women. Desire is the feeling of wanting to have sex. Many people think that the sexual response starts with desire, which leads to arousal and orgasm. However, some research suggests that women’s sexual responses are more complex. For example, physical desire may not occur until after sexual activity has started. Often, a woman is motivated to have sex to feel close to her partner or to show her feelings. Many women also report that they do not have to have an orgasm to feel satisfied from sex.
Arousal is the name given to the physical and emotional changes that occur in the body as a result of sexual stimulation. The following physical changes occur during arousal in women:
- Blood pressure, heart rate, breathing, and temperature increase.
- Parts of the vulva, such as the labia and clitoris, fill with blood and become sensitive.
- The vagina lubricates and expands
Arousal prepares a woman’s body for the physical act of sexual intercourse. A common consequence of lack of arousal is vaginal dryness, which in turn can lead to pain during sex. (Vaginal dryness also may be caused by hormonal changes, which is discussed later). Using a lubricant to provide the vaginal lubrication needed for intercourse may be helpful if you have vaginal dryness (see “What You Can Do”).
Sexual response difficulties can occur for many reasons. The following reasons are among the most common:
- Your state of mind—Sexual response is closely linked to your state of mind. Emotions such as fear, guilt, shame, embarrassment, or awkwardness about having sex may make it hard to relax. When you cannot relax, arousal is difficult, and pain may result. Stress and fatigue can affect your desire to have sex. Feelings for your partner also affect desire and arousal. If you are having relationship problems, they may interfere with your sexual response. A common relationship issue is a mismatch between partners in their level of desire for sex.
- Medications—Many medications can reduce sexual desire. These include antidepressants and medications used to treat high blood pressure and migraines. Drugs that act against androgens, such as the injectable birth control method, some birth control pills, and some drugs used to treat endometriosis, may reduce desire and arousal because androgens play a role in the sexual response. Pain medications also can reduce sexual desire.
- Medical and surgical conditions—Some medical conditions can indirectly affect sexual response. These conditions include arthritis, diabetes, cancer, and thyroid conditions. Some women who have had surgery find that it affects their body image.
- Your partner—Your partner may have problems with erectile dysfunction (inability to achieve or maintain an erection) or premature ejaculation (the release of semen before a man or his partner wishes it). These problems can make you anxious about having sex. If your partner is taking a drug for erectile dysfunction, he may have delayed orgasm, which can cause long, painful intercourse.
Gynecologic Problems
Pain during sexual intercourse can be a warning sign of many gynecologic conditions. Some of these conditions can lead to other problems if not treated.
Vulvar Pain
Vulvar pain can be classified as either acute or chronic. Acute pain usually goes away once the underlying condition is treated. Chronic pain lasts longer. Chronic pain also occurs in people in whom no underlying condition can be found.
Acute Vulvar Pain. A common cause of acute vulvar pain is a condition called contact dermatitis. This condition is a reaction to an irritating substance, such as perfumed soaps, vaginal sprays, douches, or lubricants. It may cause a rash, swelling, and redness. The most common symptoms are itching, burning, and pain. Treatment of contact dermatitis includes stopping the use of the irritating substance. Medications that are applied to the skin may be helpful. In severe cases, oral medication may be prescribed.
Other causes of acute vulvar pain include infections, skin disorders, and injuries. Infections can cause pain, itching, and irritation. Skin disorders may result in ulcers or cracks in the vulvar skin. Infections usually can be treated with medications. Treatment of skin disorders depends on the type of disorder. Some are autoimmune disorders that are treated with special types of medications.
Chronic Vulvar Pain. Chronic vulvar pain that has no other cause is called vulvodynia. Almost 1 in 5 women may feel this kind of pain at some time. The pain often is described as burning, stinging, irritation, or rawness.
There are two types of vulvodynia: generalized vulvodynia and localized vulvodynia. In generalized vulvodynia, the pain occurs on a large area of the vulva. In localized vulvodynia, the pain is felt on a smaller area, such as the clitoris. With either type, pain may occur when the vulva is touched or when pressure is applied, or it may not have any relationship to touch or pressure.
When the pain is confined to the vestibule (the area around the opening of the vagina), it is called vulvar vestibulitis syndrome (VVS) or vestibulodynia. The pain occurs when the area is touched, when a tampon is used, during sex when the penis enters the vagina, during a pelvic exam, when sitting for a long time, or when tight clothes are worn. The area may become red and inflamed.
Some women with vulvodynia find relief with self-care measures. These can include wearing 100% cotton underwear, washing the vulva with water only, patting (not rubbing) the area dry after bathing, and using adequate lubrication during intercourse. If these measures do not work, treatments such as medication, relaxation exercises, and counseling can be tried. For severe cases that do not respond to other treatments, surgical treatment may be recommended.
Vaginal Pain
There are many causes of vaginal pain that occur because of sexual activity. It is important to find the right cause because treatment for each differs.
Hormonal Causes. During perimenopause and menopause, decreasing levels of estrogen may cause changes in sexual response such as slower lubrication, less vulvar swelling, or reduced length and width of the vagina. You also may have lower levels of estrogen if you have just had a baby or are breastfeeding.
If you are perimenopausal or menopausal, your health care provider can prescribe local estrogen therapy (rings, creams, or vaginal tablets) to relieve vaginal dryness. Using a lubricant during sex or a vaginal moisturizer is helpful. Another option to improve lubrication is a longer period of foreplay. You also can try sexual activities that do not involve intercourse while you are waiting for treatments to work.
Vaginitis. Vaginitis, or inflammation of the vagina, can be caused by a yeast or bacterial infection. Symptoms are discharge and itching and burning of the vagina and vulva. Vaginitis can be treated with medication once the cause of the vaginitis is found.
Vaginismus. Vaginismus is a reflex contraction (tightening) of the muscles at the opening of your vagina. The tightened muscles make it difficult or impossible for your partner’s penis to enter your vagina during sexual intercourse. Some women with vaginismus also have trouble inserting tampons or undergoing a pelvic exam. Vaginismus may cause pain, most often described as burning or stinging, when you try to have sexual intercourse. In some cases, sexual intercourse is not possible because the muscles tighten so much.
Vaginismus can be treated with different forms of therapy. Physical therapy and relaxation exercises may help stop vaginal muscles from contracting. Another treatment is a form of physical therapy that uses vaginal dilators that gradually increase in size. Biofeedback is another option, as are medications.
Perineal Pain
Women who have had an episiotomy or tears in the perineum during childbirth may have pain during sex that may last for several months. Treatments include physical therapy, medications, or surgery.
Deep Pain
Pain felt deep inside the body during intercourse may be a warning sign of an internal problem. It can have many causes:
- Pelvic inflammatory disease
- Problems with the uterus
- Endometriosis
- A pelvic mass (tumor)
- Bowel or bladder disease
- Scar tissue (adhesions)
- Ovarian cysts
- Vaginal surgery
A pelvic exam or ultrasound exam often gives clues about the causes of deep pain. Further evaluation, sometimes involving a procedure called a laparoscopy, may be needed.
What You Can Do
If you have pain during sex, you should see a health care provider. There are some self-help measures you can try to relieve pain during sex. Some involve your partner, while others can be done by you alone.
- Use a lubricant. There are many types of lubricants. Water-soluble lubricants are a good choice if you experience vaginal irritation or sensitivity. Silicone-based lubricants last longer and tend to be more slippery than water-soluble lubricants. Do not use petroleum jelly, baby oil, or mineral oil with condoms. They can dissolve the latex and cause the condom to break.
- Make time for sex. Set aside a time when neither you nor your partner is tired or anxious.
- Talk to your partner. Tell your partner where and when you feel pain, as well as what activities you find pleasurable.
- Try sexual activities that do not cause pain. For example, if intercourse is painful, you and your partner may want to focus on oral sex or mutual masturbation.
- Try nonsexual, but sensual, activities like massage.
- Take pain-relieving steps before sex: empty your bladder, take a warm bath, or take an over-the-counter pain reliever before intercourse.
- To relieve burning after intercourse, apply ice or a frozen gel pack wrapped in a small towel to the vulva.
How Your Health Care Provider Can Help
See your health care provider if you frequently have pain during sexual intercourse or if pain is severe. Many causes of painful intercourse can be treated with medication, surgery, or other forms of therapy.
You and your health care provider will work together to find the exact cause of your pain. Your medical and sexual history, signs and symptoms, and findings from a physical exam are important factors in determining the cause of your pain. Sometimes, tests are needed to find the cause.
Your health care provider may ask detailed questions about your pain. Some common questions are listed as follows:
- How long have you had pain during sex? Did it just start? Have you have pain during sex since you began having sex?
- When during sex do you feel pain? Upon entry of the penis? During thrusting?
- Is insertion of a finger or tampon painful?
- Do you feel sexual arousal during sex?
You also may be asked about medications that you are taking, whether you have any medical conditions, and past events that may affect how you feel about sex, such as sexual abuse.
A physical examination is useful in finding the cause of pain during sex. Your health care provider may gently touch specific areas of your vulva and your vagina to see if the touch causes pain. Your history and your signs and symptoms will indicate whether further tests or exams are needed.
Using all of this information, your health care provider can suggest a treatment. It may be necessary to try different treatment options until the right one is found. You also may be referred to other health care providers for further evaluation and treatment, such as a physical therapist or dermatologist (a specialist in diseases of the skin). Sex therapy may be recommended for you or for you and your partner together, even if you are receiving treatment for a medical condition. A sex therapist can help you and your partner resolve the emotional, physical, and medical aspects of a sexual problem. To find a qualified sex therapist, go to the American Association of Sexuality Educators, Counselors, and Therapists (AASECT) web site at http://www.aasect.org.
Finally…
There are many causes of pain during sex. Successful treatment depends on finding the right cause. Seeing your health care provider can help you address pain during sex. With the right treatment, sex can become an enjoyable and healthy part of life.
Glossary
Adhesions: Scarring that binds together the surfaces of tissues.
Androgen: Any steroid hormone produced by the adrenal gland or by the ovaries that promotes male characteristics, such as a beard and deep voice.
Antidepressants: Medications used to treat depression.
Autoimmune Disorder: A condition in which the body attacks its own tissues.
Biofeedback: A technique in which an attempt is made to control body functions, such as heartbeat or blood pressure.
Bladder: A muscular organ in which urine is stored.
Dyspareunia: Pain with intercourse.
Endometriosis: A condition in which tissue similar to that normally lining the uterus is found outside of the uterus, usually on the ovaries, fallopian tubes, and other pelvic structures.
Episiotomy: A surgical incision made into the perineum (the region between the vagina and the anus) to widen the vaginal opening for delivery.
Estrogen: A female hormone produced in the ovaries.
Laparoscopy: A surgical procedure in which a slender, light-transmitting instrument, the laparoscope, is used to view the pelvic organs or perform surgery.
Masturbation: Self-stimulation of the genitals, usually resulting in orgasm.
Menopause: The time in a woman’s life when the ovaries have stopped functioning; defined as the absence of menstrual periods for 1 year.
Orgasm: The climax of sexual excitement.
Pelvic Exam: A manual examination of a woman’s reproductive organs.
Pelvic Inflammatory Disease: An infection of the uterus, fallopian tubes, and nearby pelvic structures.
Perimenopause: The period around menopause that usually extends from age 45 to 55 years.
Perineum: The area between the vagina and the anus.
Sexual Intercourse: The act of the penis of the male entering the vagina of the female (also called “having sex” or “making love”).
Ultrasound: A test in which sound waves are used to examine internal structures.
Uterus: A muscular organ located in the female pelvis that contains and nourishes the developing fetus during pregnancy.
Vagina: A tube-like structure surrounded by muscles leading from the uterus to the outside of the body.
Vestibule: The space within the labia minora into which the vagina and urethra open.
Vulva: The external female genital area.
Source: acog.org
