The Pap test checks for changes in the cervix that may become cancer. If a Pap test shows these changes, the result is called abnormal. In women who have regular Pap tests, abnormal changes are almost always caught early. An abnormal Pap test result may mean that further testing and follow-up are needed.
This page explains:
- What a Pap test checks for
- The most common cause of abnormal Pap test results
- Types of abnormal Pap test results
- urther tests and possible treatments that might be done
If you have an abnormal Pap test result, talk to your doctor about what the result means and the recommended next steps.
Detecting Cervical Problems
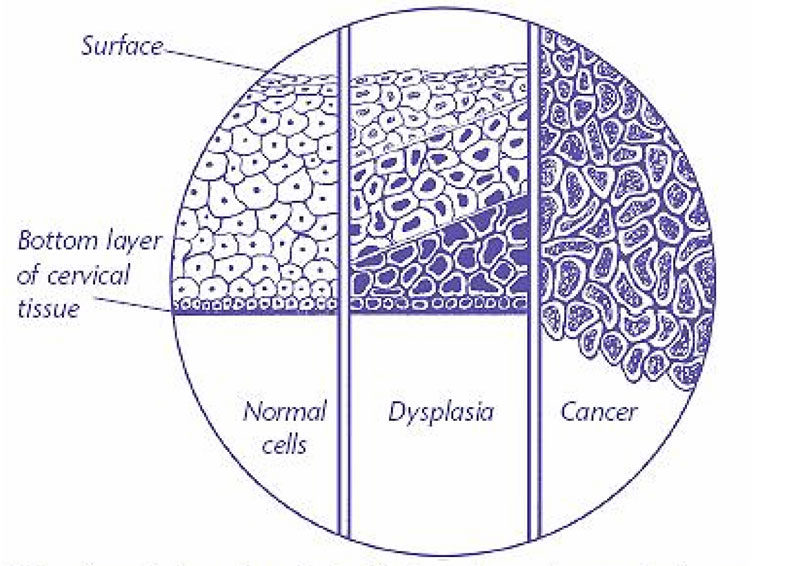
The cervix is the opening of the uterus at the top of the vagina. It is covered by a thin layer of tissue. This tissue is made up of cells. As these cells develop, the cells at the bottom layer slowly move to the surface of the cervix. During this process, some cells may become abnormal or damaged. Damaged cells grow differently. In some cases, these cells need to be removed to prevent cancer.
These abnormal cells show early precancer changes called dysplasia or cervical intraepithelial neoplasia (CIN). Dysplasia and CIN are graded as mild, moderate, or severe. Mild dysplasia (CIN 1) usually goes away on its own. Moderate (CIN 2) and severe (CIN 3) dysplasia indicate more serious changes.
The Pap test, also called a Pap smear or cervical cytology screening, checks for abnormal changes in the cells of the cervix and allows early treatment so that they do not become cancer. Regular use of the Pap test has greatly reduced the number of cases of cervical cancer in the United States.
HPV and Abnormal Pap Test Results
The main cause of abnormal Pap test results is infection with human papillomavirus (HPV). There are many types of HPV. Some types have been linked to cancer of the cervix, vulva, and vagina. Other types have been linked to genital warts.
HPV infection is very common, especially in women younger than 20 years. It is passed from person to person through sexual contact. Usually, a woman’s immune system clears the virus quickly, and the infection goes away by itself. But in some women, HPV does not go away quickly. A small number of these women will go on to develop CIN. The longer HPV is present and the older the woman, the greater the risk she will develop CIN. Smoking doubles the risk of CIN 3 when HPV is present. However, it usually takes years for precancer changes in the cervix to cause cervical cancer.
Pap Test Results: The Bethesda System
If you have an abnormal Pap test result, some of the terms used can be confusing. Most labs use the “Bethesda System” to describe Pap test results. This system uses the term squamous intraepithelial lesion (SIL) to describe precancer changes. “Squamous” refers to the type of cells that make up the tissue that covers the cervix. With this system, your results will be placed in one of several groups:
- Normal (negative) — There are no signs of cancer or precancer.
- Atypical squamous cells of undetermined significance (ASC–US) — Changes in the cervical cells have been found. The changes are almost always a sign of an HPV infection but may indicate precancer is present.
ASC– is the most common abnormal Pap test result.US - Squamous intraepithelial lesion (SIL) — Abnormal changes are seen in the cells that may be a sign of precancer. SIL can be low grade (LSIL) or high grade (HSIL). These grades are related to the grades of dysplasia and CIN (see box). LSIL almost always indicates that an HPV infection is present, but it also may indicate mild precancer changes. LSIL is very common and usually goes away on its own without treatment. HSIL indicates more serious changes. Carcinoma in situ (CIS) is a severe form of HSIL. It is the result most likely to progress to cancer.
- Atypical squamous cells, cannot exclude HSIL (ASC–H) — Changes in the cervical cells have been found. These changes are not clearly HSIL but could be. Further testing is needed.
- Atypical glandular cells (AGC) — Cell changes are seen that suggest precancer of the upper part of the cervix or uterus.
- Cancer — Abnormal cells may have spread deeper into the cervix or to other tissues.
Terms
Cervical changes may be called a squamous intraepithelial lesion (SIL), cervical intraepithelial neoplasia (CIN), or dysplasia. SIL is used to describe Pap test results. CIN and dysplasia are used to describe the actual changes in cervical cells.
| Term | CIN | SIL |
| Mild dysplasia | 1 | Low-grade |
| Moderate dysplasia | 2 | High-grade |
| Severe dysplasia | 3 | High-grade |
| Carcinoma in situ | 4 | High-grade |
Further Testing
If you are told that you have an abnormal Pap test result, you may need further testing. The follow-up that you receive after an abnormal Pap test result depends on your age and the grade of dysplasia. Sometimes, there is more than one option for further testing. You and your
Repeat Pap Test
For some women, one further testing option is to repeat the Pap test a few months later. This may give time for the changes to go away on their own. For women 21 years and older with ASC–US, the test is given every 6 months until she has two normal results. She then can return to the routine Pap test schedule. For women 20 years and younger with ASC–US or LSIL, the Pap test is repeated in 1 year.
HPV Testing
Another option for some women is an HPV test. This test detects the presence of cancer-causing types of HPV in cervical cells. The cells used for the initial Pap test often can be tested, so a woman does not need to return to the office for another test.
Colposcopy, Biopsy, and Endocervical Sampling
Colposcopy lets your doctor look at the cervix in more detail through a magnifying device. It can detect problems of the cervix that cannot be seen with the eye alone. If an area of abnormal cells is seen, your doctor may decide that a biopsy is needed. For a biopsy, the doctor removes a small sample of tissue and sends it to a lab to be studied. Endocervical sampling also may be done. A small brush or other instrument is used to take a tissue sample from the cervical canal.
Endometrial Sampling
In this test, a sample of the endometrium (the lining of the uterus) is collected for study. Some women with an AGC result need to have this follow-up test.
Treatment
Treatment of cervical changes depends on many factors. CIN 1 usually goes away by itself. For this reason, CIN 1 in women 20 years and younger is monitored with repeat Pap tests. No treatment is needed unless there is an HSIL Pap test result. In women 21 years and older, treatment is not needed unless CIN 1 has been present for 2 years, the CIN becomes CIN 2 or CIN 3, or there are other medical problems.
Several techniques are used to treat CIN:
- Loop electrosurgical excision procedure (LEEP) — A thin wire loop that carries an electric current is used to remove abnormal areas of the cervix. LEEP usually is performed in the doctor’s office with local anesthesia. The areas that are removed are sent to a lab to be studied.
- Cone biopsy — A cone-shaped wedge of the cervix is removed for study. This procedure may be done in an operating room with general anesthesia or in a surgical center with other types of anesthesia. You should be able to go home the same day.
- Freezing — Also called cryotherapy, this technique freezes abnormal tissue, which later sheds.
- Laser treatment — In laser treatment, a beam of light destroys abnormal tissue.
Some risks, such as heavy bleeding, are associated with some forms of treatment. All treatments may affect a future pregnancy. Talk to your doctor about these risks before you are treated. You also need follow-up testing after treatment, which may involve repeat Pap tests in 6 and 12 months or an HPV test. You should also get regular Pap tests after the follow-up is done.
Finally
If you have an abnormal Pap test result, talk to your doctor about what the result means and the recomended next steps. Keep in mind that many women with some types of abnormal Pap test results do not need treatment, only follow-up testing. It is important to have regular Pap tests to detect these problems. If treatment is needed, it can be done early enough to prevent cancer before it develops.
Glossary
Biopsy: Removal of a small piece of tissue that is then examined under a microscope in a laboratory.
Cervical Intraepithelial Neoplasia (CIN): Another term for dysplasia; a noncancerous condition that occurs when normal cells on the surface of the cervix are replaced by a layer of abnormal cells. CIN is graded as 1 (mild dysplasia), 2 (moderate dysplasia), or 3 (severe dysplasia or carcinoma in situ).
Colposcopy: Viewing of the cervix, vulva, or vagina with magnification using an instrument called a colposcope.
Dysplasia: A noncancerous condition that occurs when normal cells are replaced by a layer of abnormal cells.
Endometrium: The lining of the uterus.
General Anesthesia: The use of drugs that produce a sleep-like state to prevent pain during surgery.
Human Papillomavirus (HPV): The name for a group of related viruses, some of which are linked to cervical changes and cervical cancer.
Immune System: The body’s natural defense system against foreign substances and invading organisms, such as bacteria that cause disease.
Local Anesthesia: The use of drugs that prevent pain in a part of the body.
Loop Electrosurgical Excision Procedure (LEEP): The removal of abnormal tissue (of the cervix, vagina, or vulva) using a thin wire loop and electric energy. Pap Test: A test in which cells are taken from the cervix and vagina and examined under a microscope.
Squamous intraepithelial lesion (SIL): The term used in Pap test results for abnormal growth of cells on the surface of the cervix.
Source: acog.org
