Basics
Herpes is a common viral disease characterized by painful blisters of the mouth or genitals. The herpes simplex virus (HSV) causes painful blisters, usually affecting the mouth or genital area. The anal region, eyes, and fingers are involved in some people. Herpes is a lifelong disease with no cure, but most infected people have long periods without symptoms, interrupted by only occasional outbreaks. While it is a minor, annoying problem for most people, it can be a serious disease for newborns, pregnant women, and those with immune disorders.
Severe and even fatal forms of herpes, with generalized disease and nervous system involvement, can develop in newborns or in those with immune deficiencies (such as those with AIDS or certain cancers). In rare instances, women who acquire genital herpes for the first time in late pregnancy may have a severe disease course. Antiviral medications are available that can moderate symptoms and reduce the death rate in these most serious cases.
Causes
Herpes is caused by either of two viruses that are transmitted by direct contact. Once established, the virus remains dormant in the body, and activates during times of stress. Herpes is caused by two types of herpes simplex virus (HSV): HSV-type 1 (HSV-1) and HSV-type 2 (HSV-2). Either virus can cause blisters in the mouth or genital region, but HSV-2 typically affects the genitals, whereas HSV-1 most commonly affects the mouth.
HSV enters the body through a mucous membrane or a small opening in the skin as a result of direct contact (i.e. through touching, kissing, and vaginal, oral, or anal sexual activity). Although the virus is most contagious through direct contact with herpes sores, it can also be transmitted through saliva or through skin contact with people who have no visible sores or other symptoms.
After the primary infection, the herpes virus travels along the nerves and becomes dormant within nerve cells. The virus is reactivated during times of stress, and travels back out through the same pathway, causing characteristic recurring crops of blisters.
Symptoms
Oftentimes people do not know they have a herpes infection. Herpes is usually a mild infection. Some people are unaware of any symptoms, and others may mistake minor symptoms for an insect bite or rash.
The primary episode of either genital or oral herpes often causes painful blisters and flulike symptoms [Table 1]. Symptoms of an initial herpes outbreak generally occur within two weeks after infection, and are usually more severe than subsequent recurrences. One or two crops of blisters may develop, sometimes accompanied by fever, swollen lymph nodes, and in the case of oral herpes, sores within the throat or mouth. A first outbreak of genital herpes may also involve symptoms of meningitis (headache, fever, and light avoidance) lasting for up to one week.
Genital herpes is characterized by periodic outbreaks of painful genital blisters. Blisters are often preceded by a painful or tingling sensation, which is known as the prodrome (or prodromal period). Within days, clusters of blisters appear, typically on the penis or vulva, but they can also occur elsewhere, such as on the thighs or around the anus. If the blisters develop within the urethra, you will experience difficult or painful urination. Women may also develop hidden sores within the vagina or on the cervix, and only notice vaginal discharge. Herpes blisters may join together, and usually develop into open, crusty lesions that are extremely painful and last from one to three weeks.
Genital herpes blisters appear as clusters, typically on the penis or vulva, but they can also occur elsewhere, such as on the thighs or around the anus. Herpes blisters may join together, and usually develop into painful, open, crusty lesions that last from one to three weeks.
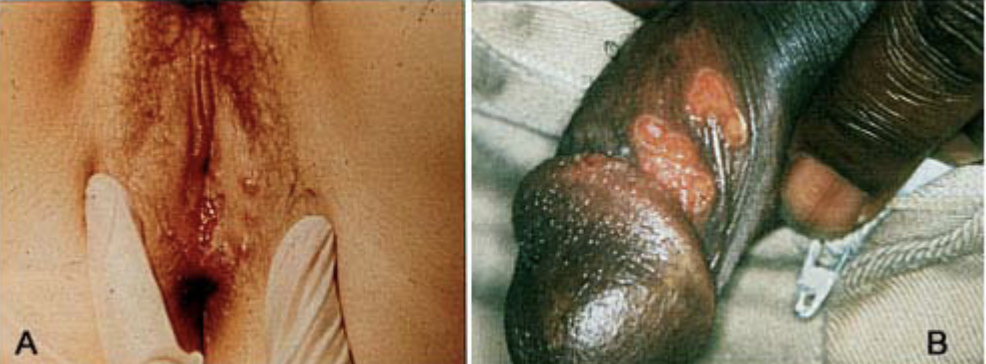
Four or five outbreaks typically occur in the first year after infection. With time, frequency and severity usually diminish, and the outbreaks may stop completely. Women usually have more severe symptoms than men do.
Oral herpes involves occasional eruptions of “fever blisters” around the mouth [Figure 2]. Often referred to as “cold sores” or “fever blisters,” characteristic herpes lesions often appear around the mouth at times of illness, after sun or wind exposure, during menstruation, or with emotional stress. Lesions can occur within the mouth, on the lips, or on the skin around the mouth.

Oral herpes lesions often appear around the mouth at times of illness, after sun or wind exposure, during menstruation, or with emotional stress. Lesions can occur within the mouth, on the lips, or on the skin around the mouth.
Blisters on the fingers or other areas occur less commonly. Sores on the fingers (known as “herpetic whitlows”) and eyes can also develop from touching one’s own or another’s sores. Eye infections can cause severe pain, blurred vision, or puffy, red and itching eyes. Usually only one eye will be involved.
In rare cases, herpes may affect the central nervous system. A herpes infection that spreads to the central nervous system (herpes encephalitis) is very serious, and must be treated as a medical emergency. If untreated, herpes encephalitis is fatal in 70% of cases. Symptoms of herpes encephalitis include headache, fever, seizures, behavioral changes, and memory loss. Acylovir is the drug of choice for herpes encephalitis, and will be given intravenously in the hospital for 10 days.
People with immune disorders often have more severe symptoms, and may develop complications in multiple organs. People who have HIV, or who are immunocompromised for other reasons often develop a more severe course of herpes. Recurring blisters, known as chronic herpetic ulcers, may be more frequent, more painful, and more prolonged.
HSV can also spread and affect multiple organs in people with immune disorders. The esophagus, lung, or liver are frequent sites of involvement. Sores in the esophagus can lead to weight loss, difficult or painful swallowing, or chest pain. Fever and yellowing of the eyes may occur if the liver is affected, and symptoms of pneumonia may be present with lung involvement. More unusual complications may be present in the adrenal glands, joints, and kidneys. Headache, fever, seizures, behavioral changes, and memory loss can develop if the central nervous system becomes involved. Women who acquire a primary herpes infection during late pregnancy can also develop more severe symptoms and complications.
Infected newborns may develop severe disease. Newborns infected during or shortly after birth may develop the characteristic blisters, redness, pain, or swelling of the eyes, or general severe illness symptoms within several days to six weeks. If the nervous system is affected, your newborn may exhibit seizures, lethargy, or show areas of paralysis.
Cases involving severe general illness of the nervous system are serious, and may lead to permanent brain damage or death. Treatment with antiviral therapy can reduce the severity of infection, and has reduced the resulting death rate to 25%.
| Primary Infection: Genital and Oral | Recurrent Outbreaks: Genital and Oral | Eye Involvement | Herpes Encephalitis | In Immunocompromised Patients | Newborns (to 6 weeks of age) |
|---|---|---|---|---|---|
| Painful blistering sores | Painful, itchy, or tingling sensation where blisters will form | Redness | Headache | Signs of esophagus involvement: pain or difficulty with swallowing | Sores |
| Fever | Painful sores | Pain | Fever | Signs of hepatitis: yellowing of eyes, fever | Infected eyes |
| Swollen lymph nodes | Swelling | Seizures | Signs of pneumonitis: cough, chest pain | Lethargy | |
| Sore throat (oral herpes) | Blurring of vision | Changes in behavior | Signs of central nervous system involvement: fever, behavior changes | Seizures | |
| Headache, light avoidance (genital herpes) | Memory Loss | Paralysis |
Risk Factors
Herpes is often acquired before adulthood. Oral herpes is usually acquired in childhood. By some estimates, 90% of adults in the U.S. have oral herpes by the time they reach their forties.
Genital herpes, which is transmitted by sexual activity, has increased significantly in the US since the late 1970s. Experts estimate that about one out of four people in the U.S. over the age of 30 are infected with HSV-2. The virus is more easily transmitted to women than men. Rates also correlate with number of sexual partners.
Having unprotected sex, or having sex with multiple partners, puts you at risk for acquiring HSV. As for any sexually transmitted disease, having unprotected sex or sex with multiple partners, and failing to use safer sex precautions puts you at risk for an HSV infection. Knowing your partner’s health status and using condoms correctly and consistently can help reduce your risk for acquiring HSV.
Newborn infection is a special risk, particularly if the mother had her first infection in middle or late pregnancy. Infants born to women who developed their first infection during mid to late pregnancy have a much higher risk of developing herpes than those born to mothers with an outbreak from a longstanding infection. The risk of newborn infection is increased in premature births if birth is delayed for a long period after membranes have ruptured. Using scalp monitors to track a fetus’s heartbeat can also increase the likelihood of transmission, as the scalp sometimes becomes punctured while electrodes are being attached. Newborns can also acquire herpes from being handled by someone with oral herpes.
Diagnosis
Health care providers can diagnose herpes by physical examination, sampling any sores present, and performing laboratory tests. It is important to distinguish herpes from other sexually transmitted diseases that can also cause genital or oral ulcers. Some of these diseases must be treated promptly to avoid serious illness.
Herpes lesions classically appear as multiple tiny blisters on a red background. Within a few days, the blisters open and join together. They are extremely painful, and may be preceded by a tingling sensation.
To confirm the diagnosis, a variety of lab tests can be run from scrapings taken from the sores. The virus can also be isolated with tissue culture.
Usually there is no need to distinguish between HSV-1 and HSV-2 infections. It can become important, however, in the case of pregnancy, to determine if an outbreak is a recurrence of an old infection, or if it is due to a primary infection with a new virus. If the latter has occurred, there is a greater danger of transmitting the virus to the newborn.
Prevention and Screening
Although they cannot offer complete protection, “safer sex” precautions provide the best prevention against genital herpes. Regular and correct use of latex condoms is recommended for preventing many sexually transmitted diseases. Because HSV can be transmitted in the absence of a sore and by contact with skin other than that of the penis, condoms can only reduce the risk and not completely prevent infection. For best protection against herpes infection with a known carrier, abstain from sexual activity when symptoms are present, and use condoms between outbreaks.
Special precautions should be taken to avoid transmitting herpes to newborns. A pregnant woman with a history of genital herpes should be examined close to the time of birth. If lesions are present, the baby should be delivered by caesarean section. If a primary infection occurs in the latter half of pregnancy, preventive medications for both the mother and the newborn should be considered.
It is also possible for babies to become infected from contact with a person with oral herpes. Therefore, anyone with oral lesions should avoid handling newborns.
Urgent Care
A physician should examine new outbreaks of genital or oral ulcers. Sexually active individuals with an outbreak of oral or genital sores and no known history of herpes should see a doctor. Other serious diseases that must be treated at once (such as syphilis) must also be considered. HIV testing is also recommended if a new sore is present. Known herpes carriers who develop an atypical sore (e.g., one that is painless) must be examined to determine if another sexually transmitted disease such as syphilis or gonorrhea has been contracted.
See a doctor at once if you suspect that your newborn may have herpes. A pediatrician should evaluate blistering sores, symptoms of eye infection, or generalized illness with lethargy or neurological signs in a newborn at once, even if the mother has no known history of herpes.
Consult a doctor right away for severe herpes outbreaks, especially if other symptoms are present. In rare cases, herpes may develop into a serious illness involving the liver, lungs, or central nervous system. In this case, you must start antiviral therapy immediately. Even if only skin sores are present, using medication may be warranted to reduce pain and shorten the duration of blisters. Those with frequent or severe recurrences should keep medication on hand to use at the first sign of an outbreak, or should consider taking daily medications to suppress outbreaks.
Self Care
Simple measures can sometimes prevent outbreaks and relieve symptoms. Applying sunscreen around the mouth before going outdoors may prevent oral outbreaks. Warm baths may help relieve painful genital lesions.
Drug Therapy
Your doctor is the best source of information on the drug treatment choices available to you.
Special Circumstances
Special precautions are needed for pregnant women with genital herpes. Pregnant women with a history of genital herpes should be carefully examined for sores at the time of labor. If lesions are visible, the baby should be delivered by cesarean section. After birth, the baby should be watched carefully for signs of infection and treated if symptoms appear. Some experts recommend that if lesions are present on the mother at the time of birth, cultures should be taken from the baby’s mucous membranes to determine if HSV was acquired.
Pregnant women who acquire an initial infection of genital herpes from mid- to late pregnancy are at special risk, both to their babies, and in rare cases, to themselves. Neonatal herpes, which is often fatal or can leave a baby with permanent brain damage, is a great risk in such cases. In rare cases, pregnant women themselves develop serious, generalized herpes from a primary infection.
HIV testing is recommended for those diagnosed with genital herpes. As risk factors involving sexual activity (having unprotected sex, or having sex with multiple partners) are the same for HIV and herpes, your doctor will likely screen you for HIV if you are diagnosed with genital herpes.
Having any open sore increases the risk of acquiring HIV from others. In addition, the herpes lesions of someone infected with HSV and HIV may contain both viruses, making transmission of both diseases more likely.
Prognosis
Herpes is a lifelong infection, but usually causes only occasional, limited outbreaks. For most people, herpes is more of a nuisance than a serious problem. Although sores are painful, outbreaks become less severe and less frequent over time. For those with more troublesome disease, antiviral medications can usually moderate or suppress outbreaks.
Pregnant women, immunocompromised individuals, and newborns may have more serious disease. People with HIV, certain cancers, or those undergoing organ transplants may have more frequent, more prolonged, or more severe recurrent outbreaks of herpes.
Their lesions may also appear to be atypical. Such patients can be more susceptible to generalized disease involving the liver, lungs, central nervous system, or other organs. Newborns and pregnant women who acquire herpes for the first time are also at higher risk for severe and generalized disease. Antiviral therapy has been effective in moderating recurrent outbreaks and reducing the death rate for the most severe cases. Neurological complications of HSV encephalitis often cause permanent damage.
Follow-Up
If you are diagnosed with genital herpes, talk with your doctor about HIV testing, safer sex practices, and how to manage herpes during pregnancy. If you are diagnosed with genital herpes, your doctor will likely test you for other sexually transmitted diseases, including HIV. In addition, herpes infection makes transmission of HIV more likely, providing additional justification for testing.
Herpes is a lifelong disease that can be transmitted to others, even in the absence of lesions. Therefore, you should abstain from sexual activity while lesions are present (when the disease is most infectious), and use condoms at all other times.
If you are pregnant and have herpes, seek counseling regarding ways to protect your newborn from infection. You should report signs of infection during pregnancy, and your doctor should check carefully for lesions during labor.
See your doctor if herpes is more than a simple, bothersome problem to you. Discuss with your doctor the possibility of treating herpes with antiviral medications. You may wish to have them on hand to moderate an outbreak, or you may choose to take them on a daily basis to suppress outbreaks. Medication is generally effective for as long as it is taken. If your medication does not work well for you, your physician may recommend a larger dose or a different antiviral drug.
Source: PDR.net
