Endometrial hyperplasia is a condition that occurs when the lining of the uterus (endometrium) grows too much. It is a benign (not cancer) condition. In some cases, however, it can lead to cancer of the uterus. Some women are at higher risk of hyperplasia.
If you are at risk or if your doctor has diagnosed hyperplasia, this page will tell you more about:
- What tests are done to find it
- How it is treated
- How to protect against it
Endometrial hyperplasia can be treated, and women at risk can take steps to protect against it.
Who Is at Risk?
Endometrial hyperplasia is more likely to occur in certain women. Those most at risk are women who:
- Are in the years around menopause
- Skip menstrual periods or have no periods at all
- Are overweight
- Have diabetes
- Have polycystic ovary syndrome (PCOS)
- Take estrogen without progesterone to replace the estrogen their body is no longer making and to relieve symptoms of menopause
The most common symptom of hyperplasia is abnormal vaginal bleeding.
Tests
If you have abnormal bleeding along with any of the other risk factors, you may need to be tested for endometrial hyperplasia. One or more tests may be required.
Ultrasound
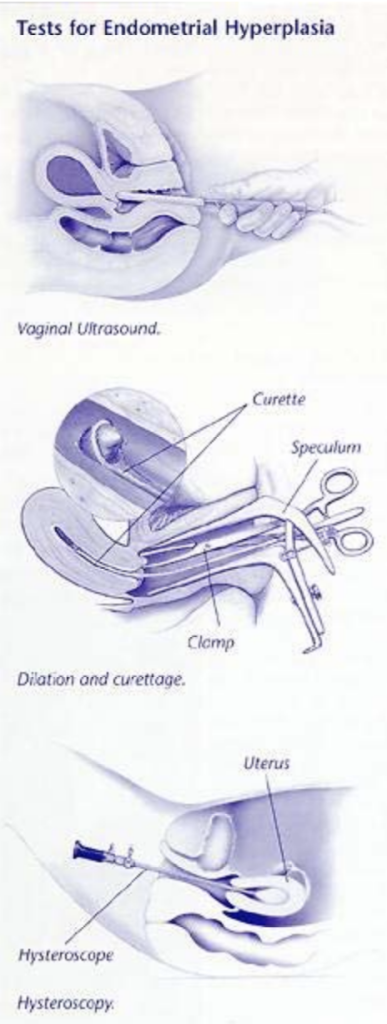
Your doctor may suggest you have a vaginal ultrasound exam. For this test, a small device is placed in your vagina. Fluid may be placed in your uterus. Ultrasound uses sound waves to make a picture of the uterine lining.
Biopsy
Endometrial hyperplasia also may be found with a biopsy of the endometrium. Endometrial biopsy can be done in a doctor’s office. Your doctor puts a narrow tube inside the uterus to take a sample of cells. You may feel some cramping during the test. The cells will be sent to a lab and checked under a microscope. Endometrial biopsy results may detect cancer of the uterus.
Dilation and Curettage
For dilation and curettage (D&C), the opening of the uterus is stretched (dilated). A special device called a curette is used to gently loosen and remove a sample of the uterine lining. This tissue then is studied in the lab to check for cancer.
You may be given anesthesia to relieve pain. It may be done in an outpatient clinic, doctor’s office, or hospital. The D&C may be done with other procedures, such as hysteroscopy.
Hysteroscopy
For hysteroscopy, your doctor inserts a slender, telescope-like device into the uterus to look for areas in the lining that may be abnormal. He or she then removes cells from these areas and sends the sample to a lab for testing.
Treatment
In most cases, endometrial hyperplasia can be treated with medication that is a form of the hormone progesterone. Taking progesterone will cause the lining to shed and prevent it from building up again. It often will cause vaginal bleeding.
You and your doctor will find a form of progesterone and a dose that is right for you. How much and how long you take progesterone depends on your condition. After you have been taking progesterone, the lining of the uterus may be tested again by endometrial biopsy.
If the problem persists, more treatment (such as other medication or surgery) may be used. Hysterectomy (surgery to remove the uterus) may be an option if you have completed your family and your biopsy showed cells that could become cancer (atypical hyperplasia). If you wish to have children, other options can be discussed.
Protecting Against Endometrial Hyperplasia
Women can take steps to reduce the risk of endometrial hyperplasia. This can protect women with certain risk factors as well as help keep it from recurring.
- If you take estrogen after menopause, you need to take a form of progesterone to reduce the risk of endometrial hyperplasia and cancer of the uterus.
- If you don’t have monthly periods, you may need to take a form of progesterone to help prevent the lining of the uterus from growing too much. Birth control pills (oral contraceptives) contain estrogen along with a form of progesterone. They may help protect against endometrial hyperplasia in women who don’t have regular periods.
- If you are overweight, losing weight may help.
The Endometrium
The endometrium is the lining of the uterus. This lining grows and thickens every month to prepare the uterus for pregnancy. If pregnancy does not occur, the lining is shed during the menstrual period.
The female hormones—estrogen and progesterone—control the changes in the uterine lining. Estrogen builds up the uterine lining. Progesterone maintains and controls this growth. At the middle of the cycle (about day 14), ovulation occurs (an egg is released from the ovary). If an egg is not fertilized, hormone levels drop. This drop triggers a normal, regular menstrual period.
As women near menopause, their bodies produce lower amounts of these hormones. After menopause, when a woman no longer has periods, very little of these hormones are produced. Some women take hormone replacement therapy to replace both hormones, or they take estrogen alone. This helps relieve symptoms of menopause.
Estrogen without enough progesterone may cause the lining of the uterus to thicken. This is called endometrial hyperplasia. In some cases of endometrial hyperplasia, the cells of the lining become abnormal. This is called atypical hyperplasia. This condition can lead to cancer of the uterus.
Finally…
In most cases, endometrial hyperplasia can be treated. Work with your doctor during treatment to prevent further problems. Women at risk can take steps to protect against endometrial hyperplasia.
Glossary
Diabetes: A condition in which the levels of sugar in the blood are too high.
Dilation and Curettage (D&C): A procedure in which the cervix is opened and tissue is gently scraped or suctioned from the inside of the uterus.
Endometrial Biopsy: A test in which a small amount of the tissue lining the uterus is removed and examined under a microscope.
Estrogen: A female hormone produced in the ovaries that stimulates the growth of the lining of the uterus.
Hormone Replacement Therapy: Treatment in which estrogen, and often progestin, is taken to relieve the symptoms caused by the low levels of hormones produced by the body.
Hormones: Substances produced by the body to control the function of various organs.
Hysteroscopy: A surgical procedure in which a slender, light-transmitting telescope, the hysteroscope, is used to view the inside of the uterus or perform surgery.
Menopause: The process in a woman’s life when ovaries stop functioning and menstruation stops.
Polycystic Ovary Syndrome (PCOS): A condition in which increased androgen causes multiple small cysts to persist on the ovaries.
Progesterone: A female hormone that is produced in the ovaries and makes the lining of the uterus grow. When progesterone decreases, menstruation occurs.
Ultrasound: A test in which sound waves are used to examine internal structures. During pregnancy, it can be used to examine the fetus.
Uterus: A muscular organ located in the female pelvis that contains and nourishes the developing fetus during pregnancy.
Source: acog.org
