During perimenopause, your periods may become less predictable. These changes are common. But some changes are not normal. Women with abnormal bleeding during perimenopause should see a health care provider. After menopause, you should not have any bleeding. A health care provider should always check bleeding that occurs after menopause.
This page explains:
- What happens during perimenopause and menopause
- How to tell if bleeding is abnormal
- Causes of abnormal perimenopausal bleeding and bleeding after menopause
- Diagnosis and treatment
Perimenopause and Menopause
Menopause is defined as the absence of menstrual periods for 1 year. The average age is 51 years, but the normal range is 45 years to 55 years.
The years leading up to this point are called perimenopause. This term means “around menopause.” This phase can last for up to 10 years. During perimenopause, shifts in hormone levels can affect ovulation and cause changes in the menstrual cycle.
How to Tell if Bleeding is Abnormal
Any bleeding after menopause is abnormal and should be reported to your health care provider. But during perimenopause, changes in menstrual bleeding are common.
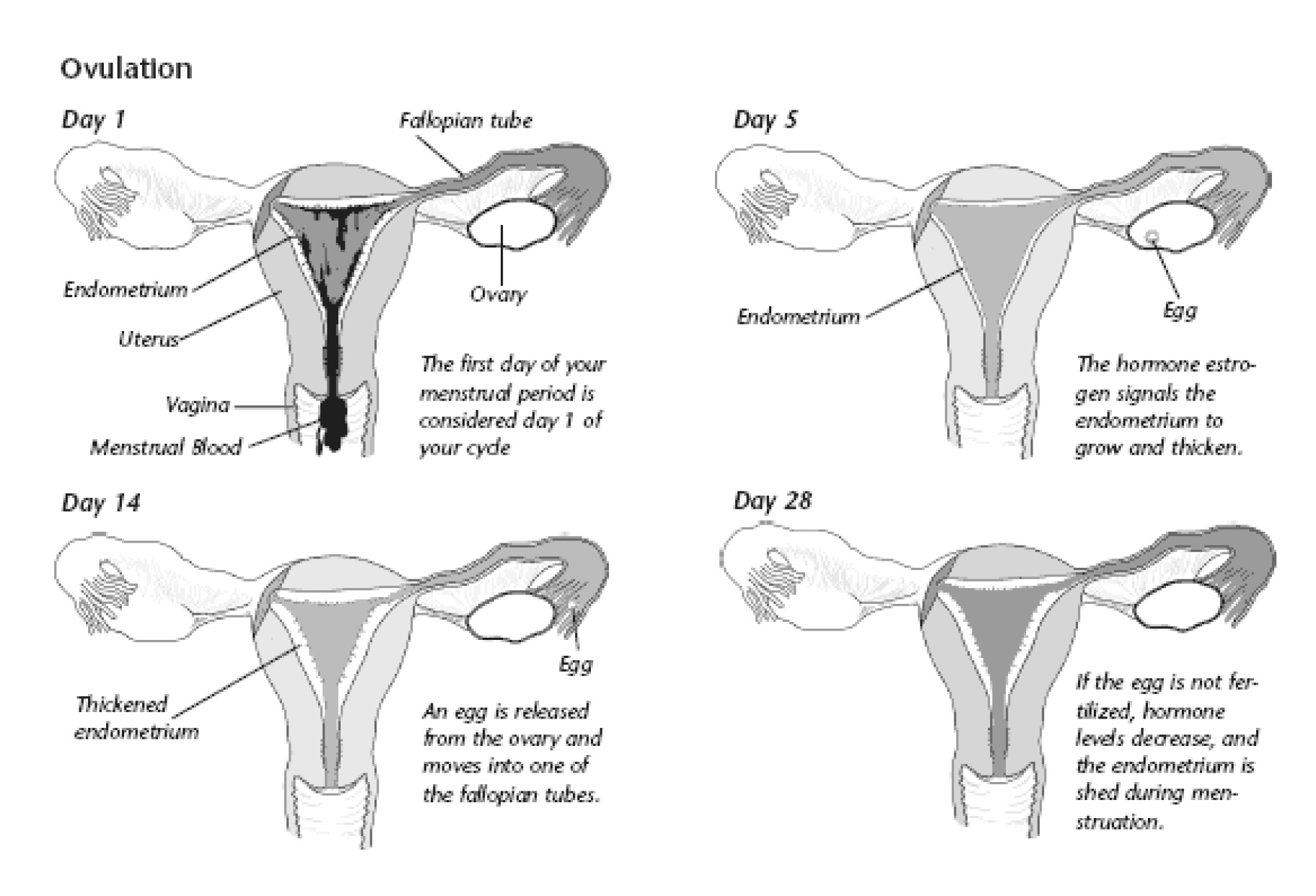
During a normal menstrual cycle, the levels of the hormones estrogen and progesterone increase and decrease in a regular pattern (see the figure). Ovulation occurs in the middle of the cycle, and menstruation occurs about 2 weeks later. During perimenopause, hormone levels may not follow this regular pattern. As a result, you may have irregular bleeding or spotting. Some months, your period may be longer and heavier. Other months, it may be shorter and lighter. The number of days between periods may increase or decrease. You may begin to skip periods.
Although these changes are normal in perimenopause, abnormal bleeding sometimes can signal a problem not related to perimenopause. A good rule to follow is to tell your health care provider if you notice any of the following changes in your monthly cycle:
- Very heavy bleeding
- Bleeding that lasts longer than normal
- Bleeding that occurs more often than every 3 weeks
- Bleeding that occurs after sex or between periods
Causes of Abnormal Bleeding
If you have any bleeding after menopause, or if you have any of the abnormal changes in your monthly cycle listed previously, it is important to see your health care provider to find out the cause. Many things can cause abnormal bleeding. Some are more serious than others.
Polyps
Polyps usually are noncancerous growths that develop from tissue similar to the endometrium, the tissue that lines the inside of the uterus. They either attach to the uterine wall or develop on the endometrial surface. They may cause irregular or heavy bleeding.
Polyps also can grow on the cervix or inside the cervical canal. These polyps may cause bleeding after sex.
Thinning of the Endometrium
After menopause, the endometrium may become too thin as a result of low estrogen levels. This condition is called endometrial atrophy. As the lining thins, you may have abnormal bleeding.
Endometrial Hyperplasia
In this condition, the lining of the uterus thickens. Endometrial hyperplasia can cause irregular or heavy bleeding. In some cases of endometrial hyperplasia, the cells of the lining become abnormal. This condition, called atypical hyperplasia, can lead to cancer of the uterus.
Endometrial hyperplasia most often is caused by excess estrogen without enough progesterone. Diagnosis and treatment of endometrial hyperplasia allows for prevention of the most common form of endometrial cancer.
Endometrial Cancer
In the United States, endometrial cancer is the most common type of cancer of the female reproductive system. Listed are some risk factors for endometrial cancer:
- Advancing age
- Early age when menstruation started or older age at menopause
- Never having been pregnant
- Irregular periods
- History of infertility
- Long-term use of medications containing high doses of estrogen
- Obesity
- Polycystic ovary syndrome (PCOS)
- Treatment with a drug called tamoxifen
- Certain ovarian tumors
- History of diabetes, high blood pressure, gallbladder disease, or thyroid disease
- Personal history or family history of certain types of cancer (such as ovarian cancer or colon cancer)
- Smoking
Endometrial cancer also can occur in the absence of any of these risk factors.
Bleeding is the most common sign of endometrial cancer in women after menopause. When diagnosed early, most cases of endometrial cancer can be treated successfully.
Other Causes
Other causes of bleeding after menopause include:
- Hormone therapy
- Infection of the uterus or cervix
- Use of some medications
- Other types of cancer
Diagnosis
To diagnose the cause of abnormal perimenopausal bleeding or bleeding after menopause, your health care provider will review your personal and family health history. You will have a physical exam. You also may have one or more of the following tests:
- Endometrial biopsy — Using a thin tube, a small amount of tissue is taken from the lining of the uterus. The sample is sent to a lab where it is looked at under a microscope.
- Transvaginal ultrasound — Sound waves are used to create a picture of the pelvic organs with a device placed in the vagina.
- Sonohysterography — Fluid is injected into the uterus through a tube, called a catheter, while ultrasound images are made of the uterus.
- Hysteroscopy — A thin, lighted tube with a camera at the end, called a hysteroscope, is inserted through the vagina and the opening of the cervix. The hysteroscope allows the inside of the uterus to be seen.
- Dilation and curettage (D&C) — The opening of the cervix is enlarged.
Tissue is scraped or suctioned from the lining of the uterus. The tissue is sent to a lab, where it is examined under a microscope.
Some of these tests can be done in your health care provider’s office. Others may be done at a hospital or surgical center.
Treatment
Treatment for abnormal perimenopausal bleeding or bleeding after menopause depends on its cause. If there are growths (such as polyps) that are causing the bleeding, surgery may be needed to remove them. Endometrial atrophy can be treated with medications. Endometrial hyperplasia can be treated with progestin therapy, which causes the endometrium to shed. Thickened areas of the endometrium may be removed using hysteroscopy or D&C.
Women with endometrial hyperplasia are at increased risk for endometrial cancer. They need regular endometrial biopsies to make sure that the hyperplasia has been treated and does not return.
Endometrial cancer is treated with surgery (usually hysterectomy with removal of nearby lymph nodes) in most cases. Discuss your options with your health care provider.
Finally
Changes in bleeding patterns during perimenopause are normal, but they should be tracked and possibly evaluated. Bleeding after menopause, though, may be a sign of cancer. If you have any bleeding after menopause, see your health care provider. The earlier the cause of bleeding is found, the better it can be treated.
Glossary
Cervix: The lower, narrow end of the uterus, which protrudes into the vagina.
Endometrium: The lining of the uterus.
Estrogen: A female hormone produced in the ovaries.
Hormone Therapy: Treatment in which estrogen, and often progestin, is taken to help some of the symptoms caused by the low levels of these hormones.
Hysterectomy: Removal of the uterus.
Lymph Nodes: Small glands that filter the flow of lymph (a nearly colorless fluid that bathes body cells) through the body.
Menopause: The absence of menstrual periods for 1 year.
Ovulation: The release of an egg from one of the ovaries.
Perimenopause: The period around menopause that usually extends from age 45 years to 55 years.
Polycystic Ovary Syndrome (PCOS): A condition characterized by infrequent or absent menstrual periods, irregular ovulation (which may result in infertility), excess hair growth, and increased androgen levels.
Progesterone: A female hormone that is produced in the ovaries and prepares the lining of the uterus for pregnancy.
Progestin: A synthetic form of progesterone that is similar to the hormone produced naturally by the body.
Uterus: A muscular organ located in the female pelvis that contains and nourishes the developing fetus during pregnancy.
Source: acog.org
