A woman’s breasts are always changing. They change during the menstrual cycle, pregnancy, breastfeeding, and menopause (when menstrual periods end). Along with these normal changes, problems can arise. Most of the problems are minor, but a few can be serious. One major problem, breast cancer, is a leading cause of cancer deaths in women. This page explains:
- Screening tests that are used to find breast problems early
- Changes that may occur in the breasts and what the changes may mean
- The breast self-exam
Most breast problems can be treated with success if found early.
If you are experiencing signs or symptoms of this issue, or have questions, you can schedule an appointment with us at our Baldwin Park office in Orlando, FL.
Your Breasts
Your breasts are made up of glands, fat, and fibrous (thickened) tissue. They respond to changes in levels of the hormones estrogen and progesterone during your menstrual cycle. Hormones cause a change in the amount of fluid in the breast. This may make fibrous areas in the breast more painful.
Your breasts also change during pregnancy, breastfeeding, and menopause. You may notice changes in your breasts if you use hormonal contraception, such as birth control pills, if you use hormone therapy (HT), or if you have breast implants.
Breast Problems in Women
Most breast problems produce only minor symptoms. Because all women are at risk for breast cancer, you should be aware of how your breasts feel. Regular breast self-exams can help. Tell your doctor if you notice any changes. Most breast problems, especially in younger women, are benign (not cancer). Common symptoms include:
- Lumps (which may be felt in one exact place or throughout the breast)
- Discharge from the nipple
- Tender areas
Benign Breast Problems
The most common problem is a benign condition called fibrocystic changes. With these changes a woman’s breast may feel lumpy and tender. Symptoms of fibrocystic changes include pain, itching, swelling, and tenderness. These symptoms often occur in both breasts.
Cysts also may occur. A cyst is a small sac filled with fluid. It can be almost any size. Often cysts will vary in size, changing with the menstrual cycle or at the time of menopause. Cysts occur most often in women aged 25–50 years. They also can occur after menopause in women who take HT.
Fibroadenomas are another common type of breast change. They are solid, benign lumps. They occur most often in young women.
Most women who have fibrocystic changes, cysts, or fibroadenomas do not have a greater chance of getting breast cancer. Still, you should always inform your doctor of any symptom of breast problems right away.
Breast Cancer
Breast cancer is the second leading cause of death from cancer in women. If it is found and treated early, most women can be cured. This is why routine breast self-exams, mammography, and checkups by your doctor are important.
Hormones and Breast Cancer
Some women worry about a link between breast cancer and the hormones that are used in oral contraceptives (birth control pills) and HT. It does not appear that oral contraceptives increase the risk of breast cancer. Women who take combined HT (estrogen and progestin) have an increased risk. The risk appears to be small, but increases throughout the time that HT is taken. If you choose to take HT, take the smallest possible dose for the shortest amount of time that works for you.
Risk Factors of Breast Cancer
Risk factors are not found in all women who have breast cancer. Many women have none of them.
Increase Risk
- Certain genes (BRCA1 and BRCA2) passed on from your parents
- Breast cancer in the family, especially mother, daughter, or sister
- Personal history of cancer of the breast, endometrium, ovary, or colon
- Older age
- No pregnancies or pregnancy later in life (aged 30 years or older)
- Early menstruation (younger than age 12 years)
- Late menopause (aged 55 years or older)
- Never breastfed a child
- Postmenopausal obesity
- Alcohol intake
- Recent hormone therapy
- Recent use of birth control pills
Decrease Risk
- Pregnancy early in life (before age 20 years)
- Ovaries removed before age 40 years
- Early menopause (before age 50 years)
Screening for Breast Problems
Screening tests are used to find a health problem early. If they are done routinely, they may detect a problem before symptoms are felt. Three of the common tests for breast problems include:
- Mammography
- Doctor’s exam of the breasts
- Breast self-exam
For the best results, all 3 tests should be done. If any 1 of these tests shows a problem it should be checked out.
Mammography
Mammography is used to examine the breast tissue by X-ray. It can find tiny lumps before they can be felt. The results of your first exam are compared with later ones to detect changes. The size of your breasts or the use of breast implants does not change the need for the test. The test is more useful in women aged 40 years and older. Older women’s breasts are less dense, so it is easier to detect lumps. Also, breast cancer is more common in older women. Women aged 40–49 years should have mammography done every 1–2 years. Women aged 50 years and older should have it done every year. If you have an increased risk of breast cancer (see box), your doctor may suggest that you have this test done more often or before age 40 years. Some women feel discomfort during the test. If you still menstruate, you may find that having your test right after your period is less uncomfortable. Sometimes your doctor may suggest a repeat test. This does not always mean that there is a problem—your doctor may just want to get a second look.
The Doctor’s Exam of the Breasts
Your doctor will examine your breasts during your routine checkups. Most women should be examined at least once a year.
A breast exam by a doctor takes only a short time. The breasts are first checked for any changes in size or shape. The doctor also looks for puckers, dimples, or redness of the skin. You should tell your doctor if you have seen any discharge from your nipples or any other changes. He or she then will check each breast for signs of a problem.
If you see a change in your breasts at any time, you should have your doctor examine them. He or she will review when you first had symptoms and how long they have lasted. Then your doctor will ask questions about your medical history to check for other factors that could point to an increased risk of breast cancer.
The Breast Self-Exam
Self-exams help you learn the normal shape and feel of your breasts. They also make it easier to notice changes (see box).
If you have felt a lump, it should be checked even if your last mammography result was normal. If your exam shows a lump or if the results are not clear, more tests will be needed.
If you have breast implants of any type, ask your doctor how to check your breasts. Be sure to check the area around the chest wall when you do your self-exam. You should do self-exams throughout your life. These exams become even more important after menopause because the risk of breast cancer increases with age.
Looking
Always do the self-exam in good light. Stand or sit in front of a mirror. Place arms at your sides. Look for dimpling, puckering, or redness of the breast skin, discharge from the nipples, or changes in breast size or shape. Look for the same signs with your hands pressed tightly on your hips an then with your arms raised d high.
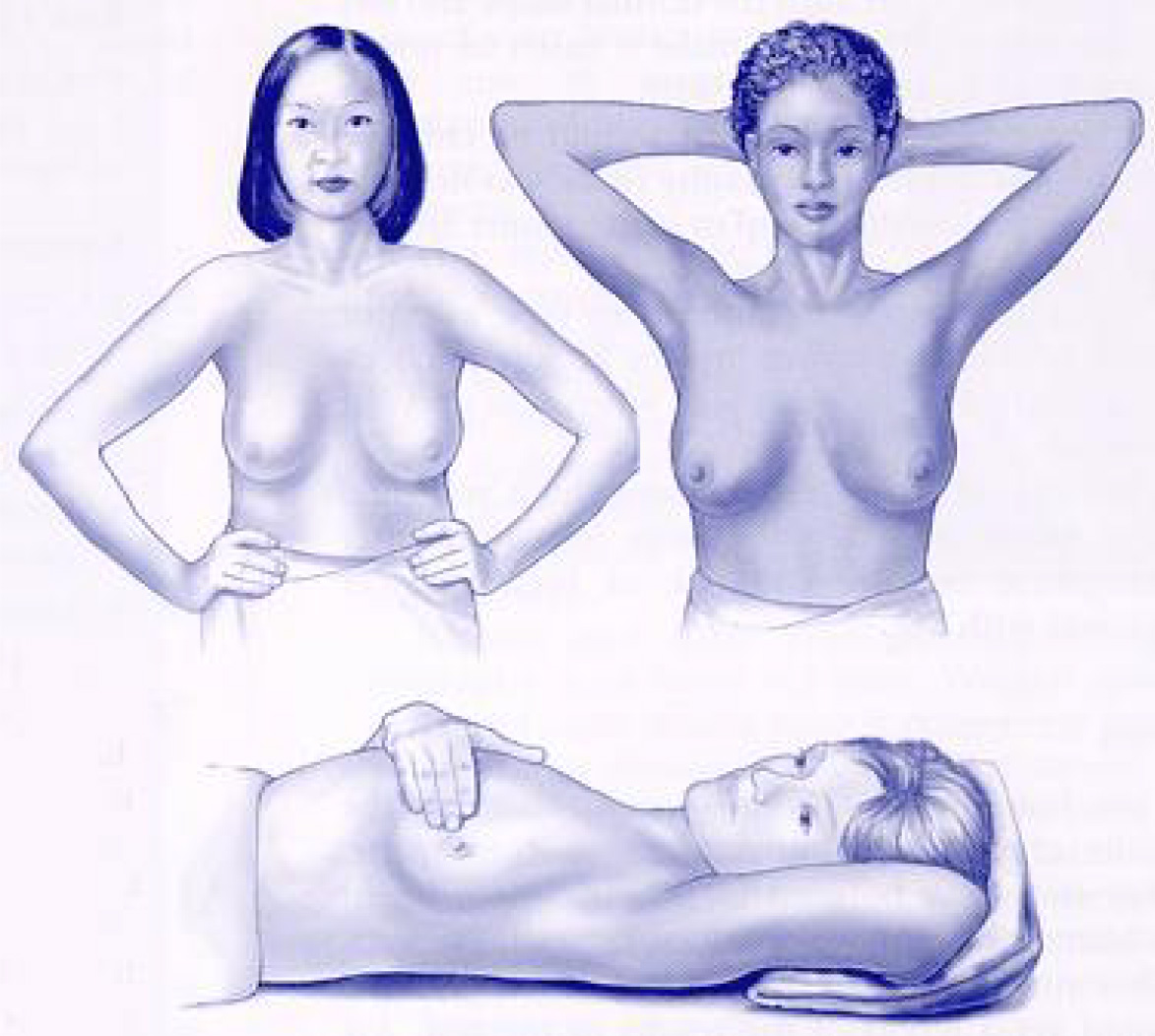
Feeling
Lie flat on your back. Place a folded towel or a pillow under your left shoulder and place your left hand under or over your head. You can also feel for changes when you are standing or when you are taking a shower or bath. It often is easier to examine your breasts when they are smooth and wet with soap and water. With your right hand, keeping the fingers flat and together, gently feel your left breast without pressing too hard. Use 1 of the 3 methods listed below. Then switch arms and do the exam on the other breast.
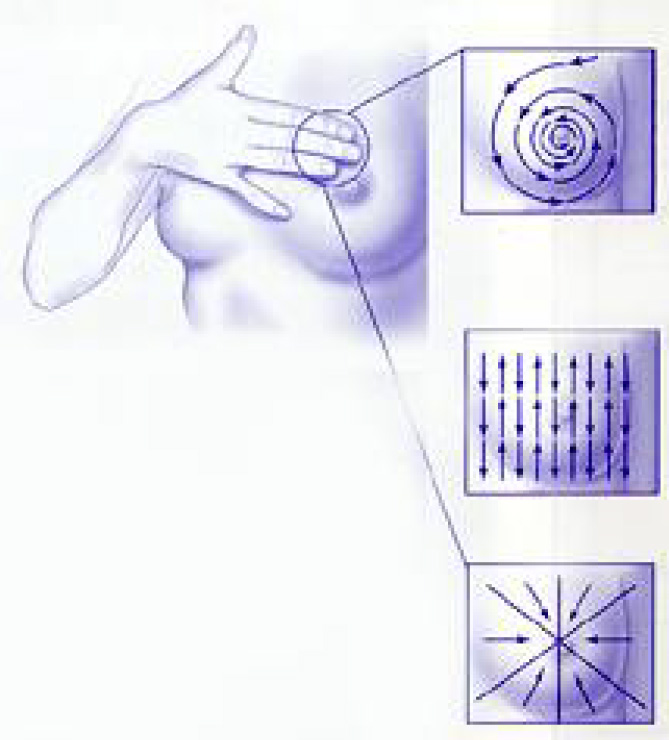
- Circle — Begin at the top of your breast and move your fingers slowly around the outside a large circle. When you return to the top, mov your hand a little closer to the nipple and make a smaller circle. Do this in smaller and smaller circles until you have examined all of the breast tissue.
- Lines — Begin in the underarm area. Slowly move your fingers down until they are below your breast. Move your fingers closer toward your nipple and go slowly back up, using the same motion. Use this up-and-down pattern a the way across your brea
- Wedge — Begin at the outside of your breast. Slowly work your way in toward the nipple, doing 1 wedge-shaped section at a time. Do this until the entire breast area has been examined.
Don’t Forget
With any pattern, be sure to examine the nipples also. Gently squeeze the nipple and check for any discharge.
Examine the upper chest area and below the armpits. These places also have breast tissue.
Call your doctor if you notice any lumps or changes in your breasts.
If you are experiencing signs or symptoms of this issue, or have questions, you can schedule an appointment with us at our Baldwin Park office in Orlando, FL.
Tests
If you have found a lump in your breast or the results of your mammogram are not complete, other tests may be used to help diagnose breast problems. Sometimes your doctor does these tests. Other times, you will be referred elsewhere. You should get a report of the results of the test. Ask your doctor about anything you don’t understand.
Ultrasonography
In ultrasonography, sound waves are used to create pictures of the inside of body organs or tissues, such as the breast. This method can tell your doctor about certain types of breast lumps. It can show whether the lumps are solid or filled with fluid, such as with a cyst.
Aspiration
Sometimes, when the doctor thinks you have a cyst, fluid or tissue is drawn through a needle to be examined. This is called needle aspiration. If the fluid is clear and the cyst goes away, it is likely that no more tests will be done. Aspiration also can be used to drain a cyst. Ultrasonography may be used to help guide the needle. The sample may be sent to a lab to be checked.

Biopsy
The only way your doctor can find out the exact nature of a lump is to study cells from it or take a sample of it. To check a solid mass or a suspicious area, your doctor may suggest a biopsy. A biopsy may be done if there is a persistent lump, even if it looks normal on a mammogram. In a fine-needle biopsy (aspiration biopsy), a small sample of cells from the mass is drawn out through a needle to be examined.
Other types of biopsy use a surgical incision (cut). Part or all of the mass may be removed.
A fine-needle biopsy often can be done in a doctor’s office. A surgical incision biopsy most often is done in a clinic or a hospital. After the breast lump is removed, cells taken from it are looked at under a microscope. Results will be negative (no cancer) or positive (cancer). Your doctor will discuss the results with you and, if needed, work out a plan for treatment. Benign breast disease often goes away on its own over time. If it does not, it often can be treated with medication or minor surgery. If you have breast cancer, it will need to be treated.
Finally
Most breast problems are benign, but breast cancer can occur. Check your breasts every month. Use this pamphlet as a guide to doing the self-exam. Visit your doctor promptly at the first sign of any problem. Follow your doctor’s advice about routine mammography. Breast problems can be treated with success if they are found early.
If you are experiencing signs or symptoms of this issue, or have questions, you can schedule an appointment with us at our Baldwin Park office in Orlando, FL.
Glossary
- Aspiration Biopsy: A procedure in which fluid or tissue within a cyst is withdrawn through a needle for study.
- BRCA1 and BRCA2: Genes that increase your risk of breast cancer and certain other types of cancer.
- Breast Implants: Sacs filled with saline or silicone gel that are placed in the breast or chest area.
- Estrogen: A female hormone produced in the ovaries that
stimulates the growth of the lining of the uterus. - Fibrocystic Changes: Formation of benign cysts and lumps of various sizes in the breast.
- Genes: DNA “blueprints” that code for specific traits, such as hair and eye color.
- Hormone Therapy (HT): Treatment in which estrogen, and often progestin, is taken to help relieve some of the symptoms caused by the low levels of hormones produced by the body.
- Mammography: A procedure in which X-rays of the breast are used to detect breast cancer.
- Progesterone: A female hormone that is produced in the ovaries and makes the lining of the uterus grow. When the level of progesterone decreases, menstruation occurs.
- Ultrasonography: A procedure in which sound waves are used to examine internal structures. During pregnancy, it can be used to examine the fetus.
Source: acog.org
